Shaping the Path Forward:
The Evolution of POCUS in Acute Cardiac Care

Dr. Hatem Soliman-Aboumarie
Consultant in Cardiac Intensive Care

Luke Baldwin
VP of Global Marketing, EchoNous
Luke Baldwin, VP of Global Marketing at EchoNous, recently spoke with Dr. Hatem Soliman-Aboumarie, a distinguished cardiothoracic intensive care consultant in London, UK, about his passion for point-of-care ultrasound (POCUS) education, training, and research. In this enlightening conversation, we explore his journey, the spark that ignited his interest in ultrasound, and the potential for POCUS to improve the quality of care delivered to patients across the healthcare industry.
[Note: This interview has been edited for clarity and brevity.]
Background and Passion for Point-of-Care Ultrasound
Luke Baldwin: Dr. Soliman, it’s great to meet you. Thank you for taking the time to speak with us. First, can you tell us briefly about your background?
Hatem Soliman-Aboumarie, MD: I work as a cardiothoracic intensive care consultant in London, UK. I’m very passionate about point-of-care ultrasound education, training, and research. This has been my passion for the last 15 years. I started my primary critical care training in Alexandria in my home country, Egypt, in 2005. In the very first years of my critical care training, I got into echocardiography. I chose it to be my primary area of research back then in Alexandria. It has continued to be my lifelong mission.
I realize day by day how important echocardiography and point-of-care ultrasound can be for improving the quality of care delivered to our patients. It can inspire people in the team to be more valuable at the bedside. So, it’s not just improving the quality of care, but it’s an important motivator for the team. When I say the team, I don’t only mean the medical team, I mean the multidisciplinary team broadly. My mission for the last few years has been to upskill the wider multidisciplinary team members.
I work at Harefield Hospital, a major quaternary cardiothoracic specialist center in the UK and Europe, internationally renowned for conducting the first combined heart and lung transplantation in Europe and for being the largest heart and lung transplantation center in the world in 1990s. Our specialization in heart and lung makes point-of-care ultrasound fundamental to our work.
Over the past few years, I’ve established a program to train the team—junior doctors, nurses, and physiotherapists—in point-of-care ultrasound. I started with lung ultrasound, considering it the most basic domain in ultrasound, easiest to learn and get accredited in with a steep learning curve and great value to patient care at the bedside.
Some of our team members have recently become accredited by the Focused Ultrasound in Intensive Care (FUSIC) national accreditation in the UK. In addition to being a clinician at the hospital, I am also the clinical lead for organ donation, which is another area of interest and passion for me.
I also have an academic role teaching point-of-care ultrasound at King’s College London. We started offering this program two years ago through the intercalated BSc program and aiming to make it more integrated within the undergraduate curriculum. I am also a board member and councilor for echocardiography at the European Association of Cardiovascular Imaging of the European Society of Cardiology with which I have been actively involved for the past ten years.
Luke Baldwin: You are a busy man!
Hatem Soliman-Aboumarie, MD: Maybe I’m busy, but it’s my passion. Look, you know, when you have something you love to do, you don’t think about the time, you just keep doing it.
Luke Baldwin: So, you said ultrasound is your passion. Can you share your origin story with ultrasound?
You started with it quite early in your medical career, so what sparked your interest and led to your passion for it? Many people in medicine encounter ultrasound, but not everyone dives in as you did. What was your introduction to it, and why did it ignite your passion?
Hatem Soliman-Aboumarie, MD: This resonates with a personal experience that sparked my interest. It all started with going with my dad, a cardiac patient, for regular echocardiograms. I was fascinated by seeing the images and the Doppler, listening even to the sounds of Doppler, and seeing how this very non-invasive thing can see a lot of structures.
When I started my critical care training at Alexandria University, Echocardiography wasn’t part of critical care training in my institution yet I was so keen on learning, I faced a lot of challenges having a very small, old ultrasound machine which was left in the stores and needed repair. And more importantly I had difficulty in finding a mentor.
Then I had this crazy idea of doing a master’s degree in critical care echo during my training, which was very novel back then in the Arab World. I was initially laughed at because people thought I was doing something unrealistic. Some told me that I chose a difficult pathway, therefore it would take me ages to find mentorship and finish my training in echo as well as my research degree. Back then, echocardiography was mostly restricted within the domain of cardiology practice and echocardiography outpatients. Nevertheless, I didn’t give up, and I kept asking mentors around until one day, the doors opened, and I got the opportunity to learn echo from one of the great masters of echocardiography in Egypt.
My master’s degree in critical care echo was conducted to study chronic obstructive pulmonary disease (COPD) patients using transthoracic echo and it involved hundred patients. Due to the challenging nature of imaging these patients, I ended up scanning almost 300 patients because many were excluded based on imaging quality. This significantly honed my skills in transthoracic echo.
Afterwards, I was unsure about the next step. But, as they say, doors open if you keep believing and going forward. Back then, I had a passion for education, so I attended a structured teaching program to improve my teaching skills, which proved very beneficial.
While working for a few years in the United Arab Emirates, I got actively engaged with the European Society of Cardiology. From there, step by step, my interest in education deepened. I began teaching locally, then nationally, and eventually internationally.
Over the last ten years, I’ve lectured in almost 60 countries worldwide, delivering talks, symposia, and webinars. While it feels like I’m still at the beginning, looking back, I acknowledge that I was very fortunate to learn something new. Now, I increasingly realize the importance of using echocardiography in intensive care, particularly as we witness the revolution in point-of-care ultrasound in acute care and emergency and critical care practice.
Integrated POCUS: Advancing Patient Care through Comprehensive Point-of-Care Ultrasound
Luke Baldwin: Many people, especially in the early 2000s, were diving into ultrasound training. Your expertise is in critical care medicine, right?
Hatem Soliman-Aboumarie, MD: My primary training is in critical care, but I also did a post-graduate Diploma in Cardiology and the American National Board of Adult Echocardiography as I was aspiring to become a cardiac intensivist.
Luke Baldwin: So, when you come across people learning ultrasound today, how do you find it? Convincing them of the value of ultrasound nowadays is easier. When students approach you for ultrasound learning, is it generally accepted, or do you still have to make a case for its value in your teaching role?
Hatem Soliman-Aboumarie, MD: It’s becoming less emphasized than before. The cultural shift is gradual. A decade ago, I had to advocate extensively for the importance of ultrasound. Now, I discuss it less, focusing more on governance, regulations, training, and accreditation. Most people I talk to understand ultrasound’s significance. However, challenges persist, primarily in regulations and the ongoing cultural shift. This extends to other specialties like nephrology, with a growing advocacy for ultrasound. I advocate for multi-specialty and multidisciplinary integration, acknowledging the inevitability of technological advancement. Miniaturized devices, now capable of complex functions, are changing the landscape. I emphasize supporting learners from non-cardiology backgrounds to prevent unstructured learning avenues like YouTube and other online resources without proper structured training. Viewing this as a positive wave for the betterment of patients, teaching provides clarity and structure.
The perception of point-of-care ultrasound has evolved from a basic exam performed by beginners to a complex assessment by experienced practitioners performed in a targeted manner in a short period. This shift is driving a change in the accreditation paradigm. I’m committed to advocating for structured training, recognizing that the journey is not easy but a collaborative process that we must embrace to improve patient care.
Luke Baldwin: That’s a fascinating distinction. I never considered it that way. In the early days of point-of-care ultrasound, it focused on specialized basic exams, addressing specific questions. However, as time progressed, it became more advanced. For instance, transesophageal (TEE) ultrasound-guided resuscitations was traditionally not an emergency medicine device. The power of ultrasound unleashed creativity, leading to new and more specialized use.
Hatem Soliman-Aboumarie, MD: Absolutely. Patients are now dealing with more complex issues, requiring beyond the binary classic point-of-care ultrasound. We need calculations and measurements—a more intricate approach. I perform complex focused assessments, especially in mechanical circulatory support. We recently published a book, “The Cardiopulmonary Point-of-Care Ultrasound,” highlighting these various aspects. The book’s concept underscores that POCUS can be basic, intermediate, or advanced. Ultrasound means you are assessing at the bedside in a targeted manner to answer specific clinical questions, ranging from very basic to very advanced.
Luke Baldwin: You mentioned calculations and specificity, moving beyond a simple yes or no. Is it safe to say that basic POCUS might be sufficient in specific patient populations, but in complex cases like the ones you handle, a more comprehensive approach is necessary?
Hatem Soliman-Aboumarie, MD: Absolutely. Different patient cohorts present unique challenges. In general intensive care units, sometimes basic POCUS might suffice. While in cardiac intensive care units, complex assessments are often required. In our unit, I often aim for complex assessments—looking at perfusion, cardiac output, congestion and pulmonary vascular resistance. This requires advanced technology and specialized devices for accurate measurements, emphasizing the evolution and adaptability of point-of-care ultrasound.
Luke Baldwin: It’s fascinating to see the evolution of technology and the acceptance of point-of-care ultrasound in diverse ways. However, on the flip side, there’s a growing sicker population with complex cases. In your experience, is the shortage of cardiac sonographers contributing to the rise of point-of-care ultrasound in acute care settings?
Hatem Soliman-Aboumarie, MD: It’s crucial to distinguish between diagnostic echocardiograms performed by cardiac sonographers and the point-of-care assessments performed by the bedside clinician. They serve different purposes. POCUS is never a replacement for comprehensive echocardiograms. Point-of-care ultrasound is an extension of bedside physical examination, providing immediate information for clinical management decisions.
Luke Baldwin: I appreciate the clarification. The focus is on targeted exams to enhance bedside examinations and guide clinical decision-making. How does ultrasound fit into the larger picture of medical advancements and innovation, and what should ultrasound manufacturers keep in mind to support this growth?
Hatem Soliman-Aboumarie, MD: The concept of point-of-care ultrasound is about targeting to enhance bedside physical examination. Ultrasound should be viewed as the true stethoscope, not just a new technology. It is crucial in triaging patients, deciding on care levels, and providing information during critical times like the COVID pandemic. As technology evolves, ultrasound manufacturers should focus on creating systems that address real-world problems, making assessments more accurate, faster, and user-friendly. Listening to clinicians’ needs and challenges will be driving advancements that positively impact patient care.
A few weeks ago, I read the biography of Professor Magdi Yacoub, the renowned surgeon who worked at Harefield Hospital, establishing it as the largest heart transplant center in the world in the 1990s. In his biography, he emphasized that the ability to innovate and push boundaries back then was due to less governance compared to what we are having today, which led them to pursue groundbreaking procedures like the first combined heart-lung transplantation in Europe. Therefore, he acknowledged that such innovations might face more obstacles today due to increased regulations, which are indeed crucial for patient safety but they are potentially stifling progress. Reflecting on this, I see point-of-care ultrasound, particularly Kosmos, as a revolution in bringing advanced concepts to the bedside. It’s a safe and powerful way to improve patient care without invasive interventions. While regulations are essential, we should balance them for meaningful progress.
Luke Baldwin: It’s fascinating to consider the historical context and the potential impact of point-of-care ultrasound. It seems like a crucial tool in advancing patient care, and you’ve mentioned the importance of training other clinicians. Could you elaborate on how you train nurses, physiotherapists, and other team members in point-of-care ultrasound?
Hatem Soliman-Aboumarie, MD Absolutely. I’m very proud of my team, and my aim is to train all of the team in point-of-care ultrasound as the enhanced modern version of the stethoscope. We’ve started a training program for junior doctors, physiotherapists, nursing staff, advanced critical care practitioners and critical care outreach. We’ve also established governance frameworks and standard operating procedures for our physiotherapy lung ultrasound to ensure safe practices and the data we collected so far showed that lung ultrasound has a strong positive impact on guiding decision-making by physiotherapy in cardiothoracic critical care.
Luke Baldwin: So, you had this trip to Kazakhstan, and I was reading something you had posted on it, and you were talking about integrated POCUS in your post when you were talking about your trip to Kazakhstan. Could you share what that trip was about and what you mean by integrated POCUS?
Hatem Soliman-Aboumarie, MD: Yeah. So, we were invited to deliver a workshop to a university hospital in Astana. Later, we got another invite to provide another workshop at another cardiac center in Almaty, one of the two main cities in Kazakhstan.
It was our first trip to Central Asia. It was terrific, not only because we were impressed by the culture and the hospitality but also because we had a fantastic setup, and they needed more similar kinds of contributions, especially point-of-care ultrasound. The workshops were very successful. We trained over 80 doctors from both cities. We even performed bedside assessments in the intensive care unit in one of the hospitals they asked us to go to, which was a critical moment because you’re not just giving a lecture, you’re applying what you do at the bedside for rea patients. I had the same feeling in my unit when I applied this every day. It is fundamental. It changes the management; it gives important insights. We applied the integrated approach, which is not only cardiac ultrasound but also the pyramid of point-of-care ultrasound. It combines cardiac, lung, and systemic venous ultrasound. So, you bring the three main pillars of point-of-care ultrasound together to assess patients’ hemodynamics, fluid status, and filling pressures. And that’s what I do in my patient cohort every day. I apply this as a protocol, and it takes around 10 to 15 minutes to perform the targeted protocol. It adds much to my information, knowing more about my patients and guiding fluid management, inotropes, and vasopressors. And that’s why I’m advocating for the integrated approach, combining cardiac, lung, and systemic venous ultrasound.
Integrating POCUS and the Advantages of Handheld Devices
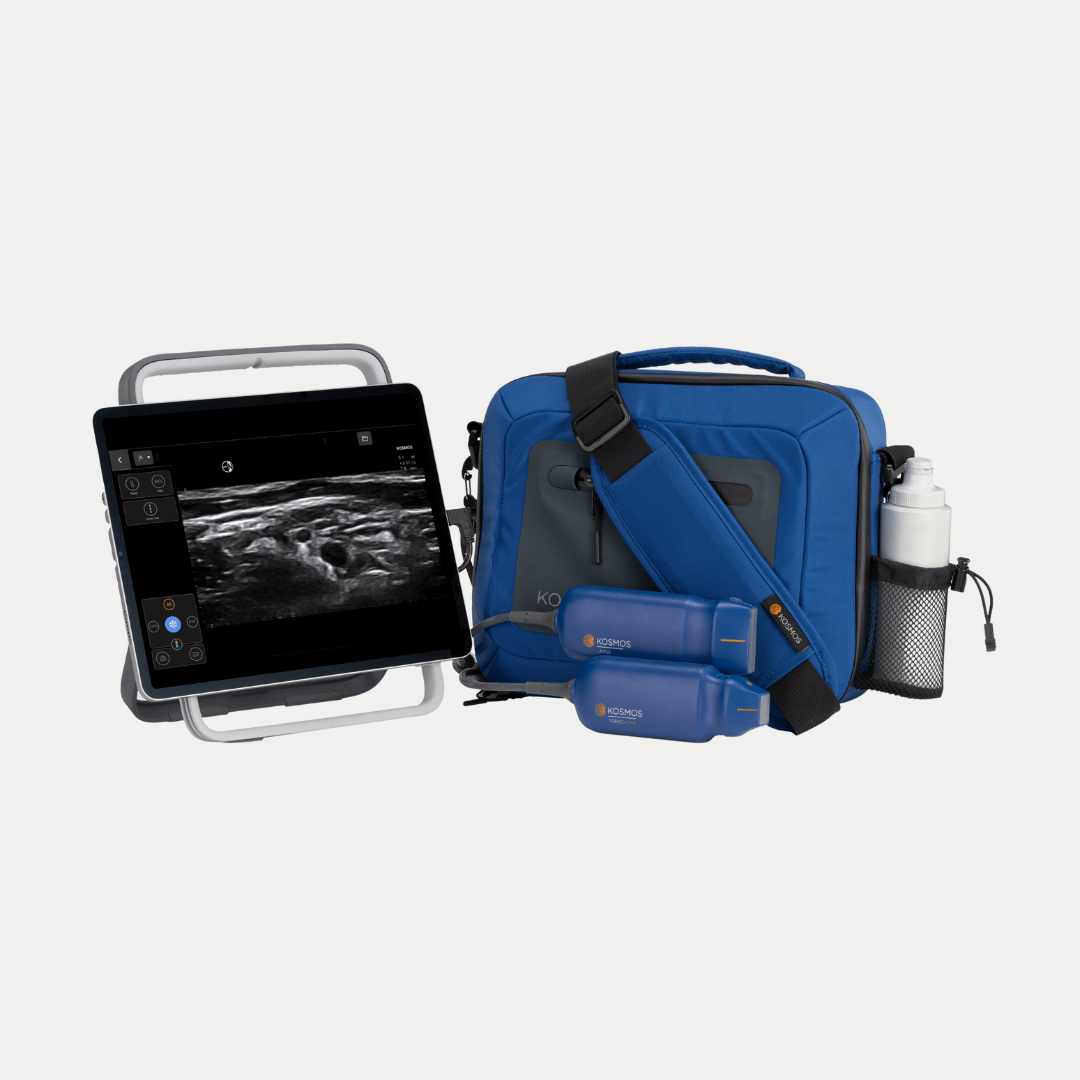
Luke Baldwin: That sounds like a meaningful and impactful trip. The integrated POCUS approach combining various ultrasound pillars seems crucial for a comprehensive patient assessment. As we’re nearing the end of our conversation, I’d like to ask about Kosmos. You mentioned you appreciate the Kosmos product. What specifically stands out about Kosmos, aligning with your goals and preferences?
Hatem Soliman-Aboumarie, MD: It’s an interesting story. Few years ago, I saw a clip on LinkedIn about Kosmos with continuous Doppler capabilities, and it blew my mind as I always I wanted a point-of-care ultrasound system with advanced Doppler assessment capabilities. The day after seeing the clip, a Kosmos representative reached out to me on LinkedIn and then I had the Kosmos system within a week. It’s so far the only handheld device in the world that brings advanced concepts like continuous and tissue Doppler in a miniaturized handheld form. There’s no other device with these capabilities, and it has been instrumental and useful in my patient care as well as teaching activities..
Luke Baldwin: That’s an incredible story of how your interest aligned with the Kosmos capabilities, leading to a meaningful connection. It’s clear that Kosmos has brought innovative and unique features to handheld ultrasound devices. I appreciate your insights into the technology and your positive experiences with Kosmos.
Hatem Soliman-Aboumarie, MD: Absolutely. Kosmos has excelled in focusing on innovation and productivity within a handheld device. It’s a pioneering idea, and this type of innovation is essential in advancing technology.
Luke Baldwin: It’s encouraging to hear your positive thoughts. When I joined, I was amazed by the capabilities, especially continuous wave Doppler and tissue Doppler on a handheld device. What are the advantages of having these features on a handheld device compared to larger clamshell products?
Hatem Soliman-Aboumarie, MD: Absolutely, it’s about convenience and efficiency. I want to be able to perform continuous wave Doppler and tissue Doppler at the bedside and even in remote areas. Bringing these capabilities to a smaller platform is the natural progression of technology. Back then, the only point-of-care ultrasound systems were binary and simple. EchoNous has pushed boundaries and changed the ultrasound landscape by bringing innovation to a miniaturized form, and the iPad Pro is also a new brilliant platform for this. It’s not very small as it offers a larger screen and powerful capabilities.
Advanced Technologies in POCUS: The Role of AI and Innovations like Kosmos
Luke Baldwin: The advancements in handheld ultrasound technology are changing how clinicians approach patient care. You’ve mentioned the impact of AI, and it’s clear that it plays a crucial role in the present and future. How do you see AI influencing patient care, efficiency, and decision-making?
Hatem Soliman-Aboumarie, MD: AI is already part of the present, and embracing it is crucial. It enhances the learning process, making it quicker and more efficient. This efficiency leads to faster assessments, quicker decision-making, and, ultimately, better patient care. The key is to be part of this transformation and leverage AI to improve clinical outcomes.
Luke Baldwin: Absolutely, quicker assessments, more efficiency, and improved patient care. You’ve also highlighted the role of AI in education. How do you see AI contributing to medical education, and have you experienced its impact firsthand?
Hatem Soliman-Aboumarie, MD: We’ve incorporated AI into our undergraduate teaching at King’s College London, and the results have been outstanding. We trained over 100 medical students using the AI capabilities of Kosmos, and the students showed rapid learning, increased confidence, and a better understanding of anatomical parts. It’s a powerful tool for education.
Luke Baldwin: That’s impressive. It seems that AI has the potential to revolutionize medical education. It’s been a pleasure discussing how this technology is impacting medical education with you.
Hatem Soliman-Aboumarie, MD: Absolutely, education is the key. Thank you for the insightful conversation.
To learn more about Kosmos, contact us today!