Dr. Gregorio Romero González
POCUS in Daily Practice: A Nephrologist’s Perspective
Point-of-care ultrasound (POCUS) is gaining recognition and popularity as a key diagnostic tool in a variety of medical settings, from family practice to cardiology, critical care, emergency medicine, and more. Dr. Gregorio Romero González is a nephrologist and consultant.
Watch the video below, or read a lightly edited transcript of the interview below. Republished with the permissions of Dr. Gregorio Romero González. This interview is edited for clarity and readability online.
Watch the video above, or read a lightly edited transcript of the interview below. Republished with the permissions of Dr. Gregorio Romero González. This interview is edited for clarity and readability online.
Dr. Gregorio Romero González on “POCUS in Daily Practice: A Nephrologist’s Perspective”
My name is Gregorio Romero-González. I am a nephrologist at the German City Pujol University Hospital in Barcelona, Spain. I’m currently working in the Extraterritorial Therapy Unit of the Nephrology department in our hospital and also, and I am a consultant in the Cardiorenal Medicine Unit and in the Surgical Intensive Care Unit in the University Hospital.
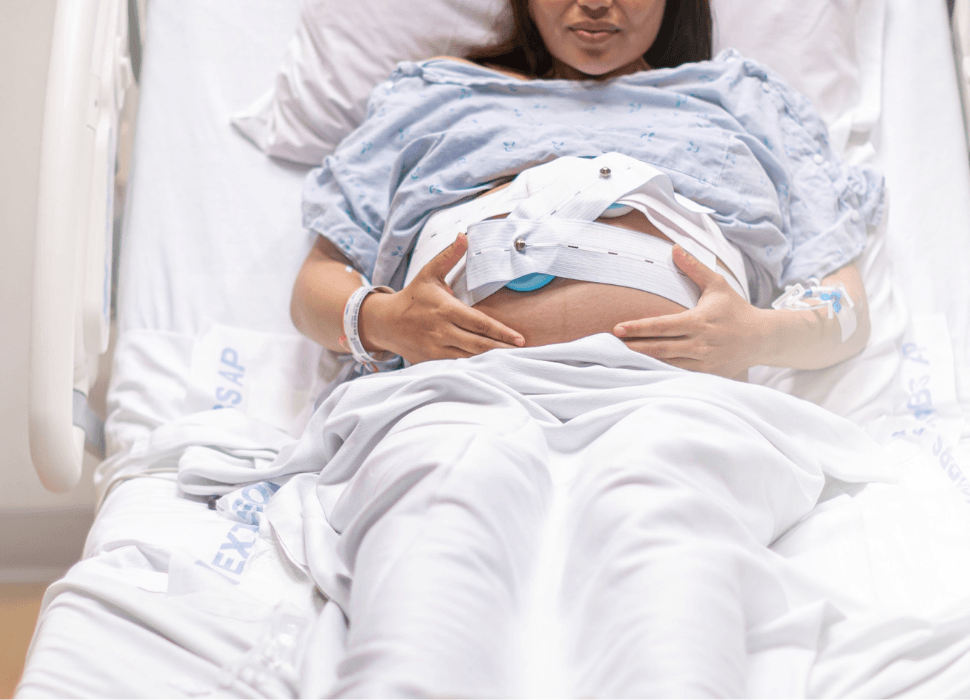
In my daily practice, we use POCUS mainly as the diagnostic tool, especially focused on the correct assessment of the volume assessment in patients on acute and chronic kidney disease.
This tool not only allows us to access the congestion, but also helps us to widen this congestive therapy. With either diuretics or extracorporeal ultrafiltration, that means that my main activity with the point-of-care ultrasonography is as a diagnostic tool in order to evaluate the congestion.
The main objective of using the point-of-care ultrasonography tool is to increase the sensitivity of the traditional physical examination. Point-of-care ultrasonography was recently called the fifth pillar in the classical physical examination. We know that we can include the information as a new tool in order to improve the physical examination and our skills in the exploration.
We use this tool in patients with clinical congestion and it’s mainly helped us to phenotype the tissue and vascular congestion. We strongly believe that the phenotype congestion helps us to initiate and personalize congestion strategies and also widen congestive therapy. I think in summary, POCUS is a precision tool in the patient with clinical signs of congestion and heart failure for example.
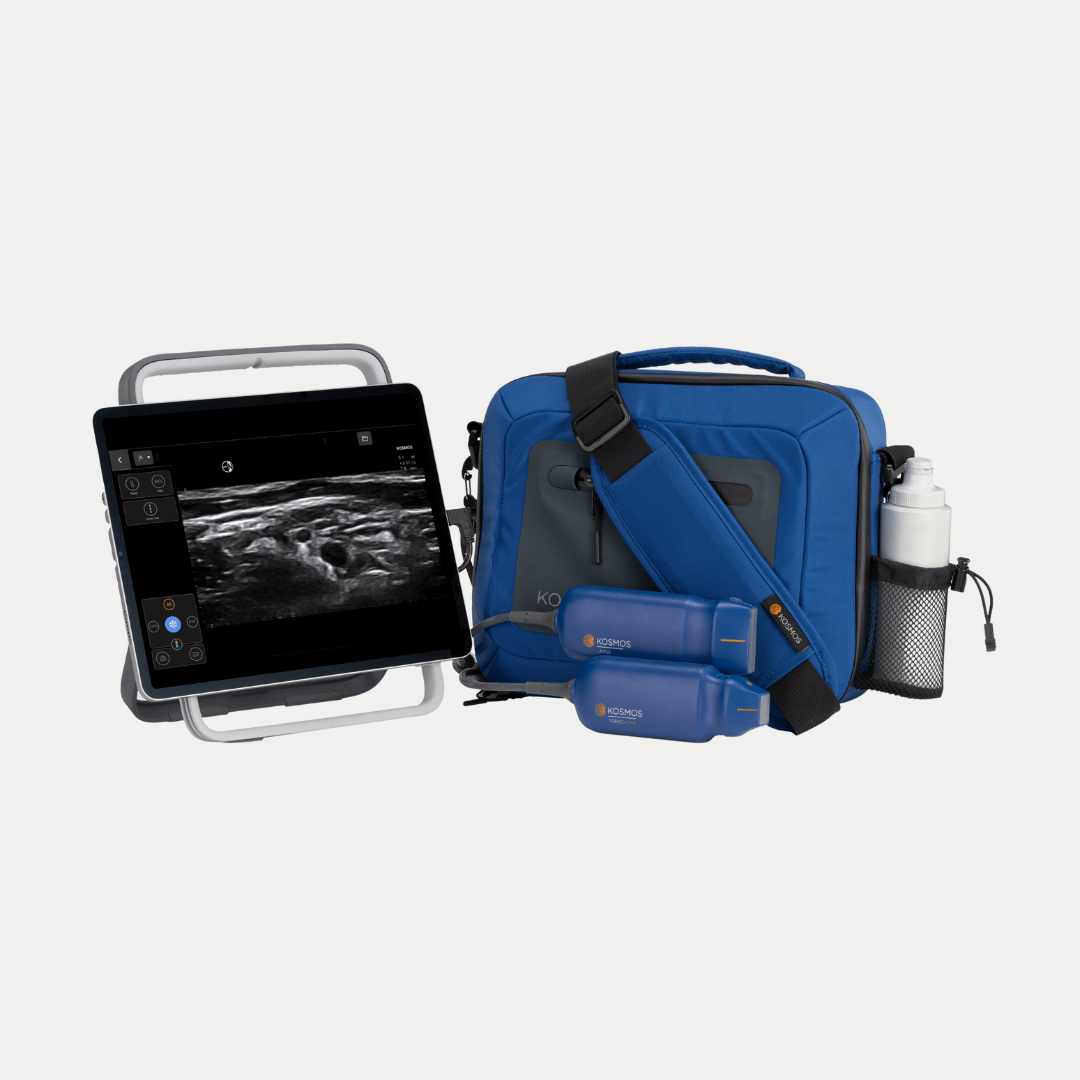
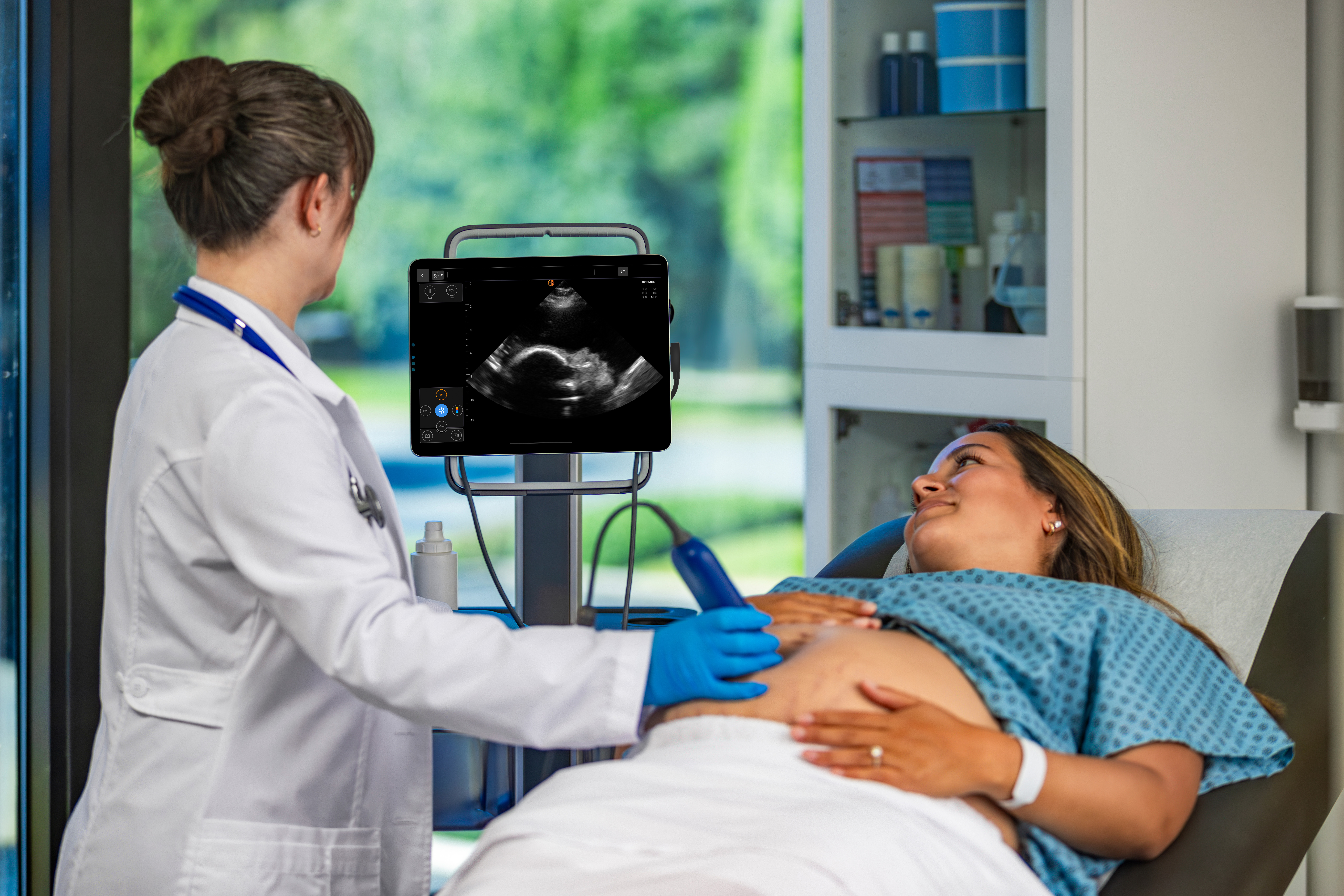
Of course, we’ll assign super portable ultrasound devices such as Kosmos for example, allow us to complete ultrasound examinations from the lung to the heart, including the examination of the abdominal organs and the assessment of the venous congestion, for example.
We can do all of these at the bedside of the patient, and I think that this is a very important skills for the ultra portable devices, because we can take the ultrasound and go to the patient and perform a correct examination at the bedside and by any clinician is not necessarily an expert in ultrasound specialty or anything. I think that any clinician, in any specialty, can perform the point of care sonography.
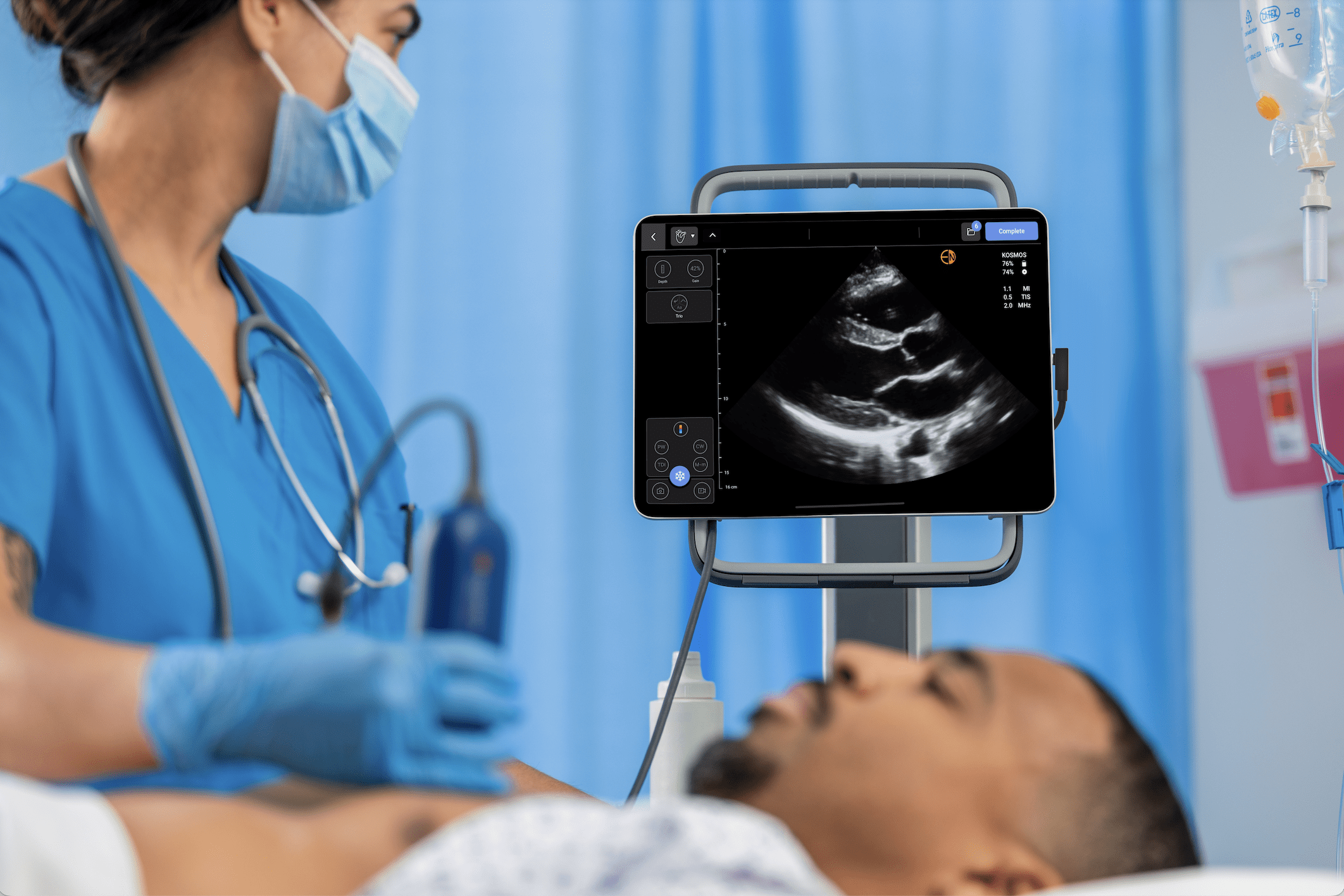
And in my opinion, the device Kosmos allows artificial intelligence to support the clinician to obtain great needs for the correct clinical integration, one of the main objectives of the point of care sonographer. In my experience, we use artificial intelligence, with the focus of cardiac ultrasound because the Kosmos machine has good skills in order to identify the correct plane in order to interrogate the heart.
Also we can obtain the correct differentiation of the different structures in the heart examination and in my opinion it is a good skill for the people that start to learn the point-of-care ultrasonography. Because artificial intelligence can assist in the correct interrogation of difficult structures, like the heart for example.
We believe that the recent incorporation of these two, although simple, can be used by any clinician at the bedside, requires basic and advanced courses. Of course, in experienced centers which cannot only certify the correct interpretation of the nations, however, all of all of these competence should be included in the training programs of the nephrology specialities and even be endorsed by scientific societies such as the Nephrologic Society, Cardiologic Society, Radiology Society.
I think that it’s important that all the specialties include the point-of-care sonography in the training programs. The main barriers could be summarized by the clinic, the clinical situation, the equipment and the professionals. As for the clinics, the main barrier is ignoring the importance of the correct assessment of the congestion. I think that the clinicians don’t have a sensitivity with the correct physical examination and the importance of increasing sensitivity to the physical examination.
For example, I often I often hear that my colleagues say it’s not necessary to do an ultrasound if the patients have oedema, but it’s not true because the patients have tissue congestion, but we don’t know if the patient has vascular congestion and for this reason it’s very important to include the point-of-care ultrasound.
It obviously is important that the Department of Nephrology and other specialties acquire the devices with the capacity to go to the patient and explode at the bedside of the patient, not with big machines in a specific place. But it’s important to go with the ultrasound to the patient. And of course it is necessary to correct certain training in the point-of-care ultrasonography, because it’s easy, we know that it’s very easy and we can do this type of techniques, but by any clinician. But it’s important that these people could be correctly training in good training centers and with experienced people that can certify these kinds of skills.
POCUS is recently adopted in our specialty, but anesthesiologists, intensivists, cardiologists have adopted this technique in the past. That is not new, these kinds of techniques, but in nephrology, I think that it is very, very important that all the nephrologists acquire this kind of competence. Because it’s the best way to improve our physical examination, we every day have patients with problems regarding congestion. And if we increase our capacity to make a correct physical examination and increase our sensitivity of the physical examination and phenotype correctly, the congestion we can, we can personally personalize the patient and we can do precision medicine that is an important concept now. In my opinion, POCUS is now the moment to include in our daily practice and is really, really important for us.