The Most Important Ultrasound Techniques for Intensivist
Ultrasound in Critical Care: Modern Intervention for Intensivist
Intensive care protocols are crucial in modern medicine; they have rapidly evolved, commanding a growing trend of global adoption. Critical care impacts care outcomes directly, resulting in lowered mortality rates and significant improvement in quality of life.
However, beyond these impacts, the numbers also speak volumes; between 2000 and 2010, the annual cost of critical care medicine in the United States averaged $108 billion, a 92% increase from an average of $56.6 billion in 2000. Also, the 2010 cost represents 13.2% of hospital costs, 4.1% of national health expenditures, and $0.72 of gross domestic product (1). By 2031, these numbers are expected to surge rapidly based on projected estimates by the Centers for Disease Control and Prevention (CDC).
Now, while the cost of critical care suggests rapid expansion, it does not exactly reflect practice effectiveness. ICU misdiagnosis and therapy failure are still heavily reported. In a BMJ Quality and Safety paper published in 2012, researchers from the Department of Anesthesiology and Critical Care Medicine, John Hopkins University School of Medicine investigated the rates of potentially fatal ICU misdiagnosis and associated clinical complications in the general population.
This observational study showed that the prevalence of misdiagnosis ranged from 5.5% to 100%, with 28% of autopsies reporting at least one misdiagnosis and about 8% identifying as a Class 1 diagnostic error. A review of multiple studies showed that vascular events (linked to inadequate imaging protocols) and infections (linked to medication failure) were the leading lethal misdiagnosis (2).
Key Takeaways:
- The global cost of critical care medicine is rapidly increasing annually; unfortunately, the upward trend also featured an increase in the annual average rates of ICU misdiagnosis
- Ultrasound modalities including POCUS offer enhanced imaging technology, precise visualizations, and AI-assisted workflows to enhance care delivery, reduce misdiagnosis rates, and offer continuous patient monitoring
- Intensivist and emergency care specialists trained in POCUS techniques stay ahead of the curve; their competencies and skills improve patient management and monitoring in all clinical settings
- Kosmos, an EchoNous solution in modern, ultraportable ultrasound, is a best-in-class tool for accurately deploying ultrasound capabilities in critical care medicine
Table of contents
- The Most Important Ultrasound Techniques for Intensivist
- Ultrasound in Critical Care: Modern Intervention for Intensivist
- POCUS in Critical Care Medicine
- POCUS Techniques in Critical Care Medicine
- Ultrasound Protocols for Intensivist: Revolutionizing Care Deliver in Critical Care
- Kosmos: A POCUS Solution for Intensivists
- Explore Kosmos for Critical Care
- References
POCUS in Critical Care Medicine
In an attempt to correct this anomaly, the Critical Care niche has received huge attention and research funding lately. In fact, multiple technological interventions in imaging and remote patient monitoring have been developed as protocols redefining the standards of care. Point-of-care ultrasound (POCUS) provides accurate imaging information for intensivist, reducing misdiagnosis errors and improving care outcomes.
Since its introduction, intensivist have widely adopted POCUS in managing critically ill patients as an emergency care or patient monitoring intervention. Compared to conventional protocols, POCUS is inexpensive, digitally enabled, and readily available; its simple integration procedures, design, and operation (often AI-enabled) ease care workflow for intensivist – even the less technologically-savvy ones.
Its immediate offerings are incredible; intensivist spend less time acquiring diagnostics images and performing measurements required for correct assessment and diagnosis. Today, POCUS complements diagnosis and treatment workflows, supplying the inputs needed to solve the problems of misdiagnosis in critical care medicine.
POCUS Techniques in Critical Care Medicine
With its wide adoption, POCUS modalities most common in intensive care medicine include basic cardiac, lung, and abdominal ultrasound.
1. Basic Critical Care Echocardiogram
The first comprehensive, modern-day description of Basic Critical Care echocardiogram (CCE) was published in the 2009 Statement of Competence in Critical Care Ultrasonography (3). This consensus statement established ultrasound modalities as a point-of-care utility tool, emphasizing a general call for adoption by emergency care specialists and intensivist. At its core, CCE answers the clinical questions focused on target-oriented quality assessments guiding patient monitoring and management (4).
Commonly, CCE modalities are performed repeatedly on the same day or subsequent days with a clinical objective of assessing the effectiveness of any ongoing medical intervention – this might include drug regimen, surgery, or physical therapy. For intensivist, the cognitive skills required (as outlined in the statement of competencies) include the capability to assess global left ventricular size and function, identification of segmental versus global wall motion abnormalities, right ventricular size and function, and identification of severe valvular dysfunction based on color Doppler.
CCE, as currently defined, captures four echocardiography views:
- Parasternal long axis
- Parasternal short axis
- Apical four-chamber
- Subcostal views
These views investigate the clinical integrity of the physiological operations controlling myocardial contractility, right ventricular dilation, left ventricular filling, and other abnormalities like pericardial effusion. Myocardial contractility (in this regard) includes regional wall motion abnormalities like akinesia, dyskinesia, and hypokinesia.
Clinical utility for the CCE views has expanded rapidly; intensivist and emergency care specialists consistently use POCUS procedures as a complementary – or alternative – diagnostics tool for clinical abnormalities not exactly captured by the 2009 Statement of Competence in Critical Care Ultrasonography.
Although not exhaustive, the table below pairs the CCE views with reported clinical utilities.
| View | Main Utility |
| Parasternal long axis | Global assessment of visible structures and function |
| Parasternal short axis (midventricular level) | Left Ventricle systolic function, segmental wall motion analysis, septal kinetics |
| Apical 4-chamber | Right Ventricle to Left Ventricle ratio |
| Subcostal long axis | Global assessment of visible structures and function |
| Inferior vena cava long axis | Assessment of volume status |
Key Features of Basic CCE
1. Echo-free space between the heart and the parietal layer of the pericardium
Space volume helps intensivist accurately assess a possible case of dyspnea, estimate the size of effusion (in diagnosed cases of pericardial effusion), and guide the characterization of pericardiocentesis. Basic CCE can detect a minimum volume of 15 mL; space volume measurements greater than 50 mL suggest pathological conditions requiring medical interventions.
2. Basic Lung Ultrasound
Modalities for Basic Lung Ultrasound in managing critically ill patients were first described in the 1990s. Many literature reviews on this subject credit Dr. Daniel Litchenstein, and describe his role in the eventual wide adoption of lung ultrasound as a basic competency for emergency care specialists and intensivist. Fortunately, the adoption cycle coincided with the emergence of low-cost, portable ultrasound technologies certified for assessing cardiac and lung abnormalities.
Today, point-of-care (POCUS) lung ultrasound offers comprehensive information that aids the clinical monitoring of a patient’s condition with little or no radiation risk – this is a huge advantage over chest radiographs, computed tomography (CT) scans, and other conventional methods.
Recently, clinical studies have supported its use in diagnosing and managing lung pathologies. Peris et al (2010), in a reference study, demonstrated how point-of-care lung ultrasound reduces the use of chest radiographs and CT scans in critically ill patients by 26% and 47% respectively (5). Beyond expanding the modalities of professional practice in critical care, POCUS also serves incredible treatment utility.
In 2014, a group of researchers from Toulouse, France published a reference study comparing the diagnostic accuracy of lung ultrasound and an integrative cardiopulmonary ultrasound approach in patients with acute respiratory failure (ARF) managed under critical care. The study pooled over 38 patients with ARF and showed that the diagnostic accuracy rates of lung ultrasound for cardiogenic pulmonary edema and pneumonia are better when paired with CCE (6).
X-ray findings in lung function monitoring (under critical care) are ambiguous, forcing intensivist to confirm and reconfirm X-ray outputs with other modalities. Observational studies have also shown that lung X-rays and auscultation are insensitive in diagnosing heart failure and pulmonary congestion; these findings further positioned point-of-care lung ultrasound as a superior diagnostic and monitoring tool in patients requiring critical interventions. POCUS modalities can also accurately identify cardiogenic or non-cardiogenic pulmonary edema (interstitial syndrome) pleural effusion, consolidations, and pneumothoraces.
Key Features of Basic Lung Ultrasound
1. A-Pattern
A-Patterns are horizontal artifacts indicating normal lung surface with an accuracy of 67% for sensitivity and 90% for specificity. Clinical utility for this feature includes the identification and assessment of dry inter-lobular septa, response to PEEP recruitment, and the diagnosis or exclusion of large pericardial effusion.
2. B-Profile
B-lines show as vertical ring-down artifacts, not fading with increasing depth and moving with lung sliding. B-lines greater than 3 indicate a pathology and more than 2 comet-tailed B-lines are indicative of thickened interlobular septa. B-lines have a sensitivity range of 97 – 98% and a specificity range of 88 – 95%. Clinical utility for this feature includes the diagnosis of hemodynamic pulmonary edema, lung tumors, pulmonary contusion, acute respiratory distress syndromes, and many other pulmonary consolidating processes.
3. Consolidation
Consolidation on lung ultrasound is identified as hypoechoic tissue with hyperechoic punctiform images. With a sensitivity range of 92 – 93% and a specificity range of 92 – 100%, consolidation features provide details in the diagnosis and monitoring of multiple lung abnormalities in intensive care patients.
3. Abdominal Ultrasound
Unlike basic and lung ultrasound where competencies, skills, and operation modalities are individually defined, abdominal ultrasound is studied in the context of integrated protocols. A commonly studied protocol is the Focused Assessment with Sonography for Trauma (FAST). Intensivists and emergency care specialists use FAST as a tool to comprehensively assess the abdominal integrity of trauma patients. FAST procedures scan the abdomen, heart, pericardial, and pleural spaces for any physiological anomalies.
Abdominal ultrasound examinations using FAST investigate the presence of free fluid in the abdominal cavity: an indication of hemoperitoneum complicated with significant abdominal injuries. FAST provides four detailed sonographic views: pericardial, perihepatic, perisplenic, and pelvic regions. Although it is almost irreplaceable in critical abdominal care, FAST is not without a few limitations. For instance, it is inefficient in detecting retroperitoneal bleeding and early, non-bleeding organ injuries.
As a modification of FAST, the extended FAST (EFAST) protocol was designed to incorporate basic lung ultrasound as an additional aid to detect pneumothoraces or hemothorax. Compared to conventional methods like CT, X-ray, and clinical chest examination, EFAST boasts of a higher sensitivity range pegged at 17.6% to 95.3% and a specificity range of 97 – 99.9%.
Abdominal point-of-care ultrasound protocols are modern game changers. With digital and AI capabilities, POCUS for intensivist offers comprehensive and accurate imaging of the bladder, kidneys, gallbladder, and abdominal aorta. In critical care medicine, these additional capabilities enhance the detection accuracy for clinical cases requiring intensive care like hydronephrosis, cholecystitis, and abdominal aortic aneurysms.
Key Features of Abdominal Ultrasound
Depending on pathology, and imaging settings like depth, contrast, and dimension, a few characteristics are immediately obvious on abdominal ultrasound outputs. Some of these features include:
- Incomplete gastric emptying indicates the presence of semi-digested food in the stomach and intestines.
- The presence of free fluid in the hepato-renal pouch indicates intra-peritoneal bleeding.
- Bladder over distention indicates acute urine retention.
Ultrasound Protocols for Intensivist: Revolutionizing Care Deliver in Critical Care
POCUS integration into routine ICU practice serves clinical purposes ranging from diagnostics to monitoring and evaluation of therapy effectiveness. Today, Intensivists and emergency care specialists consider POCUS an extension of physical examination or an accuracy check for results obtained from conventional imaging methods.
A. As an ICU Diagnostic Modality
POCUS in intensive care medicine improves the accuracy and specificity of diagnosis. In mechanically ventilated patients, CCE modalities significantly improve diagnostic yield and inform Intensivist of a need to alter or modify therapy plans. POCUS assessment of left ventricular systolic function investigates pericardial fluid collections and provides ample clinical evidence to rule out or consider an anomaly (7). Likewise, POCUS right ventricular assessments show conclusive clinical data on ventricular septal positioning and tricuspid annular plane systolic excursion.
Ultrasound examination is recommended in the evaluation of patients with clinical presentation consistent with the cardiac etiologies suggesting possible cardiac infarction or cardiac trauma. Point-of-care lung ultrasound also accurately diagnoses acute decompensated heart failure – in this case, inputs from conventional methods like physical examination, laboratory studies, and chest X-ray may be required (8).
Recently studies have investigated the use of ultrasound modalities in the resuscitation of trauma patients in critical care medicine. The clinical cases examined highlighted how POCUS integration impacts the detection and management of hypovolemic and left ventricular dysfunction and reduces the mortality risk (9). Patients with early-phase undifferentiated shock also benefit from the routine application of CCE in intensive care units; in these applications, POCUS expedites the recognition of underlying etiologies and provides baseline clinical monitoring data.
B. As a Hemodynamic Monitoring Tool
Ultrasound modalities contribute huge monitoring inputs for critical care patients. The portability and digitally-enabled interface of POCUS position it as a valuable bedside tool for hemodynamic monitoring. A 2019 meta-analysis collated clinical data from six research studies comparing the accuracy of lung ultrasound and chest radiography in the evaluation of cardiogenic pulmonary edema complicated with dyspnea in adult patients.
A statement issued by the researchers recommended CCE for patients in shock after initial fluid resuscitation to evaluate cardiac function, rule out cardiac tamponade, and then repeat as needed to assess the burden of therapies on cardiac function (10).
Critical care echocardiogram can measure cardiac output and reliably track changes. Ultrasound modalities also reliably assess fluid responsiveness doubling as an effective method to directly measure the dynamic parameters essential for functional hemodynamic monitoring. Beyond its primary capabilities in tracking changes in cardiac output, POCUS modalities directly visualize the internal structures of the heart, lungs, and abdominal sections and provide valuable clinical data to Intensivist on ventricular physiology and the need for fluid or pharmacological intervention.
C. As a Prepping Tool in Perioperative Setting
The application of ultrasound in perioperative clinical settings is rapidly gaining wide acceptance. Patients undergoing critical surgical intervention risk significant cardiovascular and pulmonary adverse events. POCUS modalities provide a continuous stream of data required to accurately decide on triage options and the best approach to reducing the risk of perioperative complications.
Emergency CCE also aids timely diagnosis of aortic dissection and acute valvular regurgitation (11). Intensivist also leverage imaging technologies on POCUS for intraoperative echocardiograms allowing continuous monitoring with post-operative scanning. In larger contexts, Intensivist also leverage point-of-care ultrasound as a response tool for evaluating low CO syndrome, cardiac tamponade, prosthetic valve dysfunction, acute RV failure, and hemodynamic instability.
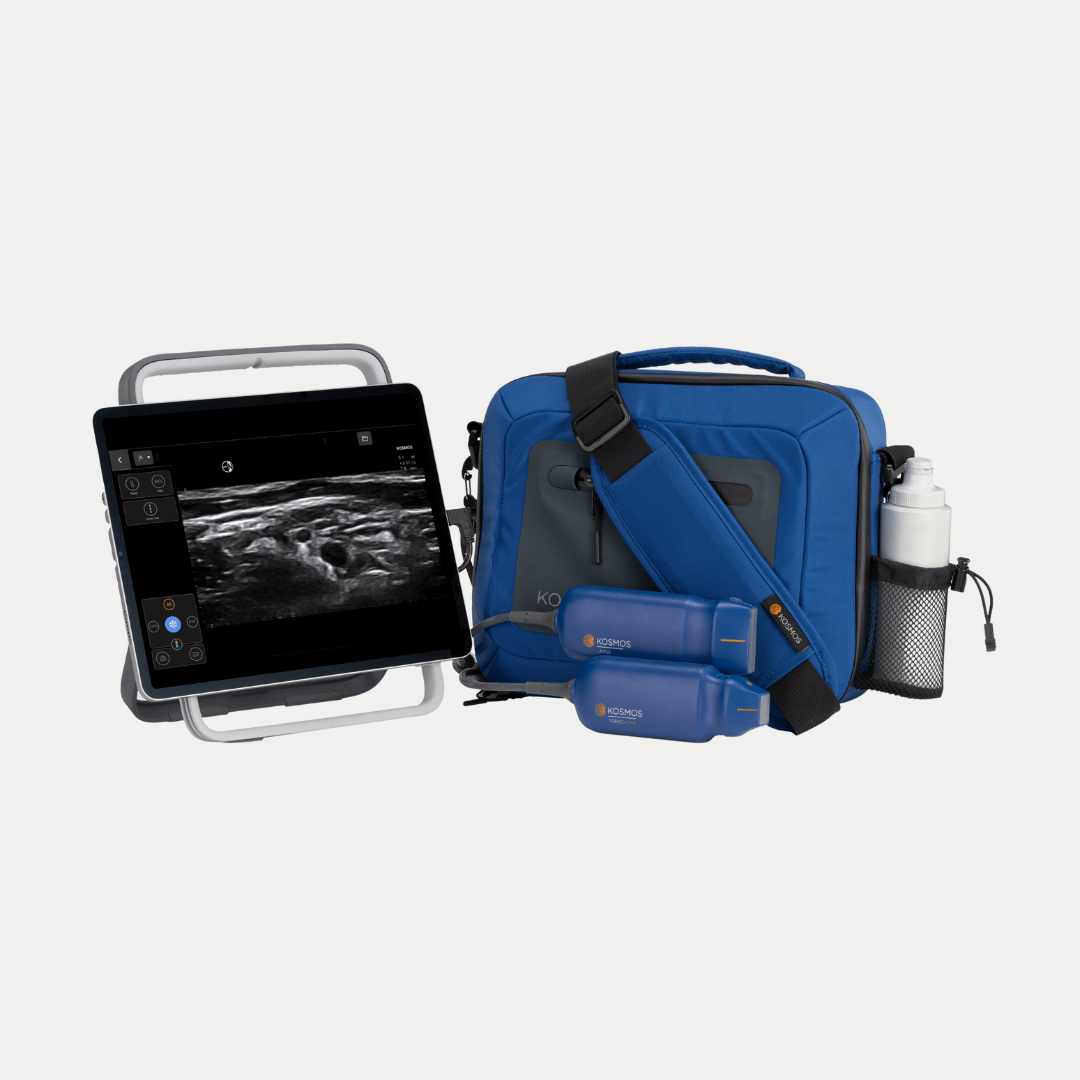
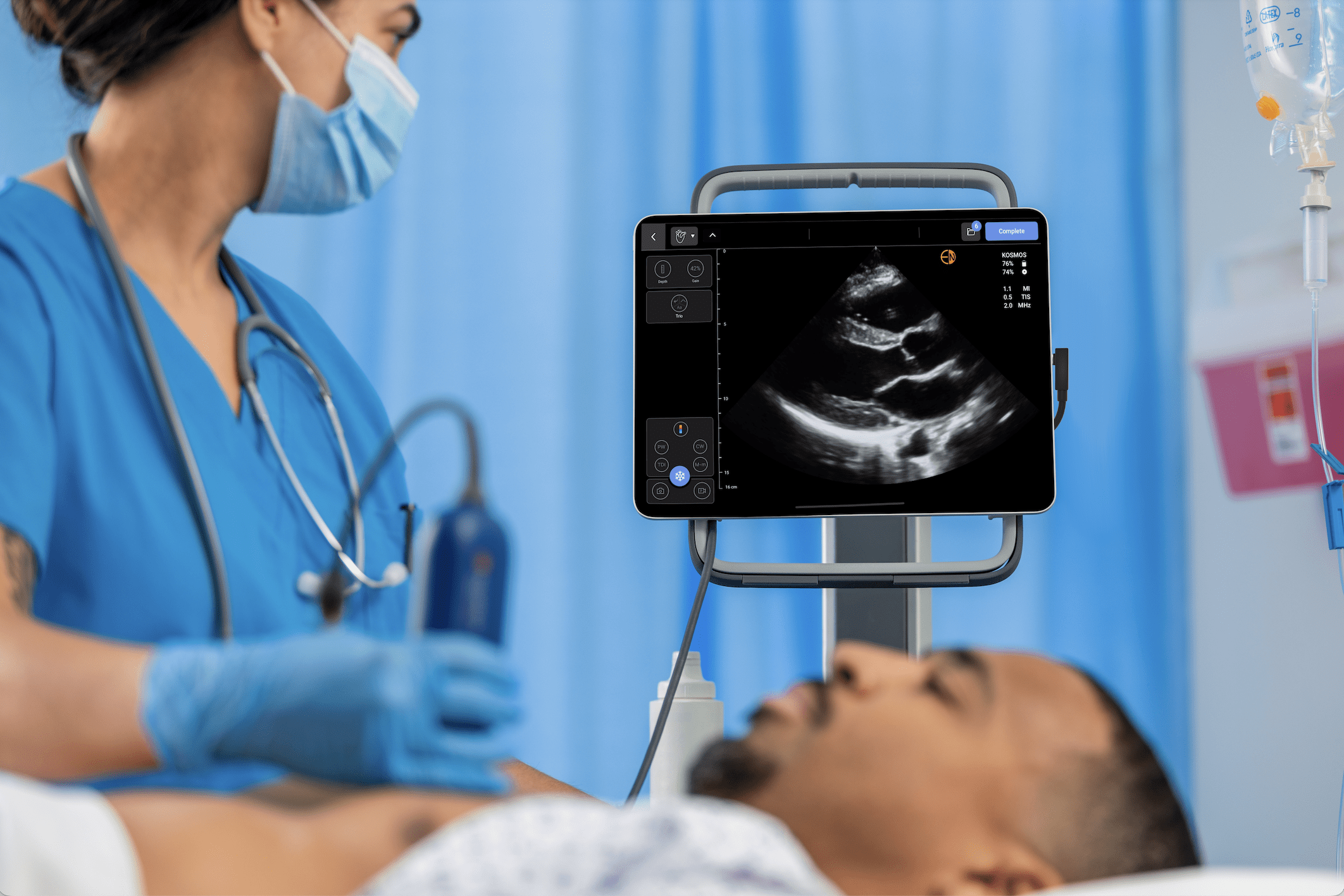
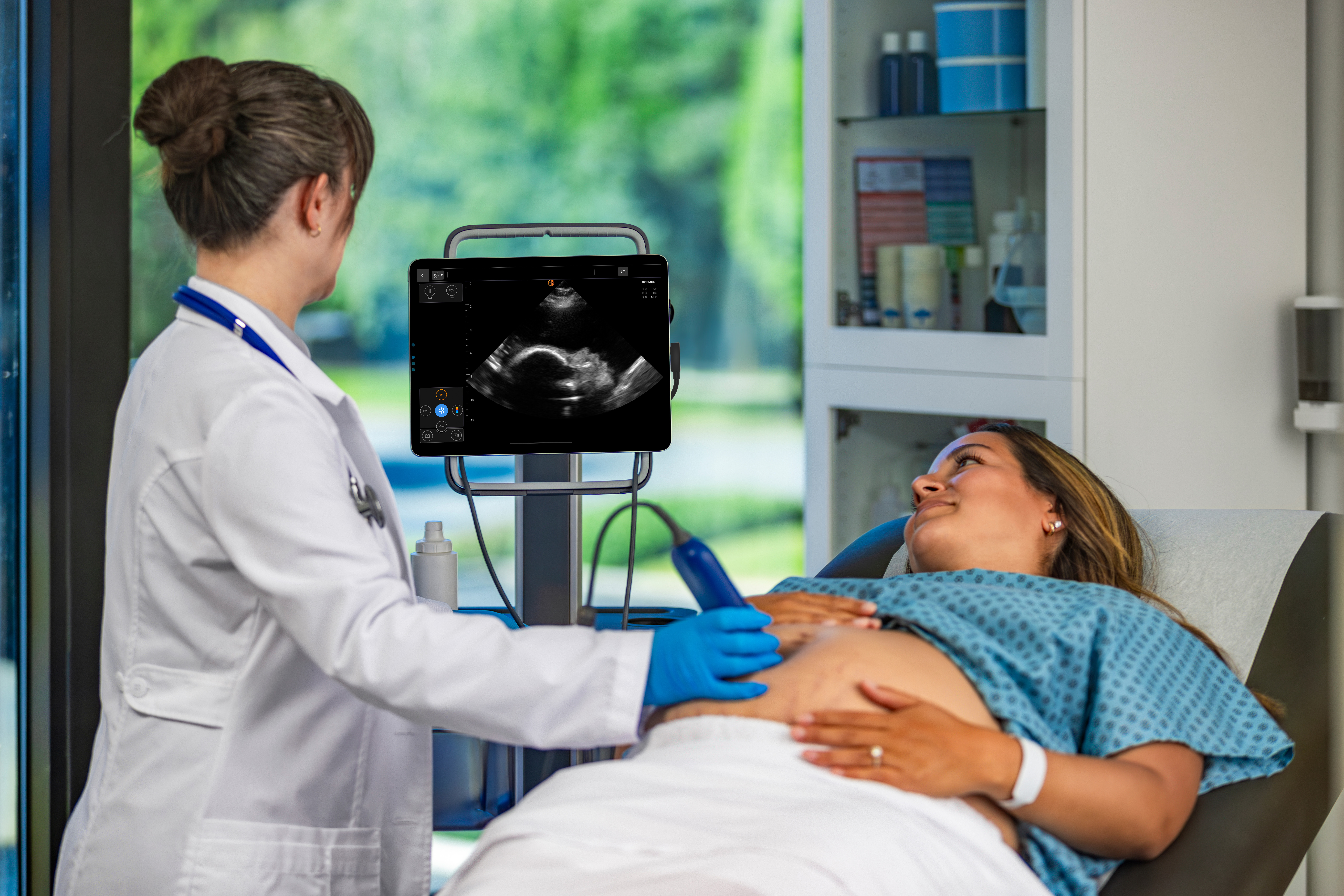
Kosmos: A POCUS Solution for Intensivists
Kosmos ultraportable ultrasound offers advanced POCUS capabilities on a level that delicately balances accuracy and versatility for critical care and emergency medicine. Its cutting-edge AI-enabled features, advanced Doppler, multiple transducers, and imaging abilities simplify POCUS integration for diagnostics and monitoring functions. With its workflow accessible entirely via tablets like iPads and Android devices, Kosmos allows multi-organ lung, abdominal, and cardiac scanning; this feature helps clinicians enhance their critical care workflow, placing the Intensivists in complete control of therapy.
AI-driven integrations are revolutionizing care delivery. Kosmos is designed with AI-assisted workflows. This capability outranks the average point-of-care ultrasound offerings on the market, placing Kosmos at the forefront of a new approach to patient care in critical medicine.
Explore Kosmos for Critical Care
Kosmos is a game-changer in critical care medicine. Enhance your ICU service with this AI-enabled ultrasound system designed to revolutionize imaging and patient monitoring. Improve your patient care offerings with a low-cost, portable solution providing exceptional Doppler capabilities and highly flexible probe configurations. Schedule your Kosmos demo today to get started.
References
- Society of Critical Care Medicine. (2024, May, 15). Critical Care Statistics. https://www.sccm.org/communications/critical-care-statistics
- Winters, B., Custer, J., Galvagno, S. M., Jr, Colantuoni, E., Kapoor, S. G., Lee, H., Goode, V., Robinson, K., Nakhasi, A., Pronovost, P., & Newman-Toker, D. (2012). Diagnostic errors in the intensive care unit: a systematic review of autopsy studies. BMJ quality & safety, 21(11), 894–902. https://doi.org/10.1136/bmjqs-2012-000803
- Lichtenstein, D., Mézière, G., Biderman, P., Gepner, A., & Barré, O. (1997). The comet-tail artifact. An ultrasound sign of alveolar-interstitial syndrome. American journal of respiratory and critical care medicine, 156(5), 1640–1646. https://doi.org/10.1164/ajrccm.156.5.96-07096
- Via, G., Hussain, A., Wells, M., Reardon, R., ElBarbary, M., Noble, V. E., Tsung, J. W., Neskovic, A. N., Price, S., Oren-Grinberg, A., Liteplo, A., Cordioli, R., Naqvi, N., Rola, P., Poelaert, J., Guliĉ, T. G., Sloth, E., Labovitz, A., Kimura, B., Breitkreutz, R., … International Conference on Focused Cardiac UltraSound (IC-FoCUS) (2014). International evidence-based recommendations for focused cardiac ultrasound. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography, 27(7), 683.e1–683.e33. https://doi.org/10.1016/j.echo.2014.05.001
- Peris, A., Tutino, L., Zagli, G., Batacchi, S., Cianchi, G., Spina, R., Bonizzoli, M., Migliaccio, L., Perretta, L., Bartolini, M., Ban, K., & Balik, M. (2010). The use of point-of-care bedside lung ultrasound significantly reduces the number of radiographs and computed tomography scans in critically ill patients. Anesthesia and analgesia, 111(3), 687–692. https://doi.org/10.1213/ANE.0b013e3181e7cc42
- Bataille, B., Riu, B., Ferre, F., Moussot, P. E., Mari, A., Brunel, E., Ruiz, J., Mora, M., Fourcade, O., Genestal, M., & Silva, S. (2014). Integrated use of bedside lung ultrasound and echocardiography in acute respiratory failure: a prospective observational study in ICU. Chest, 146(6), 1586–1593. https://doi.org/10.1378/chest.14-0681
- Via, G., Hussain, A., Wells, M., Reardon, R., ElBarbary, M., Noble, V. E., Tsung, J. W., Neskovic, A. N., Price, S., Oren-Grinberg, A., Liteplo, A., Cordioli, R., Naqvi, N., Rola, P., Poelaert, J., Guliĉ, T. G., Sloth, E., Labovitz, A., Kimura, B., Breitkreutz, R., … International Conference on Focused Cardiac UltraSound (IC-FoCUS) (2014). International evidence-based recommendations for focused cardiac ultrasound. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography, 27(7), 683.e1–683.e33. https://doi.org/10.1016/j.echo.2014.05.001
- Vignon, P., Begot, E., Mari, A., Silva, S., Chimot, L., Delour, P., Vargas, F., Filloux, B., Vandroux, D., Jabot, J., François, B., Pichon, N., Clavel, M., Levy, B., Slama, M., & Riu-Poulenc, B. (2018). Hemodynamic Assessment of Patients With Septic Shock Using Transpulmonary Thermodilution and Critical Care Echocardiography: A Comparative Study. Chest, 153(1), 55–64. https://doi.org/10.1016/j.chest.2017.08.022
- Brown, S. M., Pittman, J. E., Hirshberg, E. L., Jones, J. P., Lanspa, M. J., Kuttler, K. G., Litwin, S. E., & Grissom, C. K. (2012). Diastolic dysfunction and mortality in early severe sepsis and septic shock: a prospective, observational echocardiography study. Critical ultrasound journal, 4(1), 8. https://doi.org/10.1186/2036-7902-4-8
- Maw, A. M., Hassanin, A., Ho, P. M., McInnes, M. D. F., Moss, A., Juarez-Colunga, E., Soni, N. J., Miglioranza, M. H., Platz, E., DeSanto, K., Sertich, A. P., Salame, G., & Daugherty, S. L. (2019). Diagnostic Accuracy of Point-of-Care Lung Ultrasonography and Chest Radiography in Adults With Symptoms Suggestive of Acute Decompensated Heart Failure: A Systematic Review and Meta-analysis. JAMA network open, 2(3), e190703. https://doi.org/10.1001/jamanetworkopen.2019.0703
- Mayo, P. H., & Koenig, S. (2020). Advanced Critical Care Echocardiography Certification: An Update. Chest, 158(1), 48–49. https://doi.org/10.1016/j.chest.2020.02.037