Enhancing Patient Safety in Labor and Delivery with Point-of-Care Ultrasound
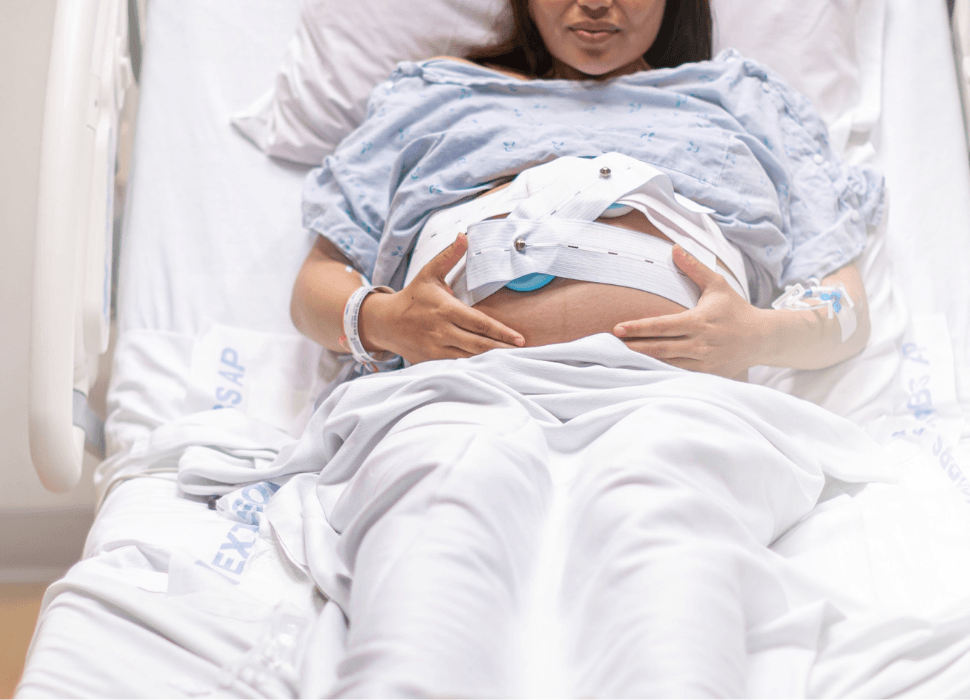
In the high-stakes environment of a Labor & Delivery (L&D) unit, information is the ultimate currency. For decades, clinicians have relied on digital cervical exams to assess cervical dilation, a subjective process with inaccuracy rates ranging from 20% to 70%1 as well as to assess fetal head position, station, and malposition alongside external fetal monitoring to guide the journey from admission to push.
However, the limitations of digital exams are not trivial: misidentification of fetal presentation or position can delay necessary intervention, contribute to prolonged labor, and increase the risk of both maternal and neonatal morbidity.
A paradigm shift is occurring. Point-of-care ultrasound (POCUS) is moving from a specialized “rescue” tool to a routine adjunct, what many are calling the “sixth vital sign” of obstetric care.2 By bringing cart-level imaging quality to the bedside in a portable format, systems like Kosmos are helping clinicians “see beyond” their fingertips, improving safety for both parent and child.
Table of Contents
- Enhancing Patient Safety in Labor and Delivery with Point-of-Care Ultrasound
- Precision in Progress: Beyond the Digital Exam
- Navigating the “Slow Progress” Plateau
- Supporting Safer Neuraxial Anesthesia
- Gastric Assessment and Aspiration Risk
- Postpartum Vigilance: Scanning for Retained Products of Conception
- The Kosmos Advantage: Cart-Level Power at the Bedside
- Summary: POCUS Applications in Labor & Delivery
- References
- Additional References
- Q&A: Enhancing Patient Safety in Labor and Delivery with Point-of-Care Ultrasound
Precision in Progress:
Beyond the Digital Exam
The most critical challenge in labor management is often determining the fetal lie, presentation and position relative to the uterus. While digital palpation has been the traditional standard, it is notoriously subjective, particularly when the fetal head is not in an ideal position.
Identifying Malpresentation Early
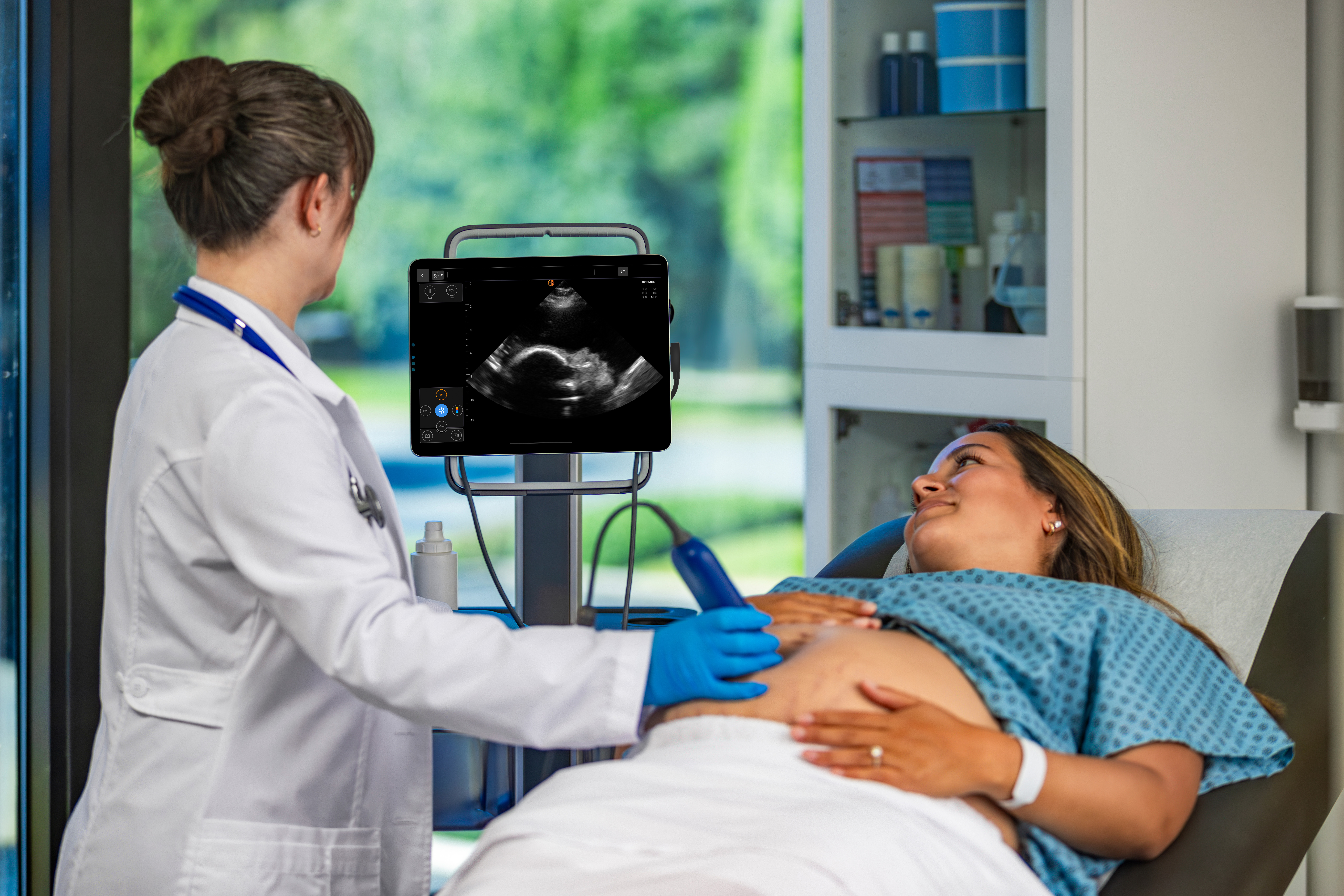
Current guidelines from the The International Society of Ultrasound in Obstetrics and Gynecology (ISUOG) recommend that ultrasound at admission is an integral component of the intrapartum assessment.3 Studies have consistently demonstrated that ultrasound-based assessment is more accurate and reproducible than digital examination for determining fetal head position, particularly for occiput presentation.4,5 Using transabdominal ultrasound, clinicians can rapidly confirm:
Fetal Position: Differentiating between occiput-anterior and the more challenging occiput-posterior (OP) positions. Occiput-posterior presentation is associated with a significantly increased risk of cesarean delivery, prolonged second stage, and instrumental delivery.4 Further, data has shown that fetal head position is determined inaccurately in almost 1 in 2 cases (with 20% remaining incorrect during instrumental delivery), increasing the risk of complications by an order of 1.46.6
Head Station and Attitude: Determining how far the head has descended and its degree of flexion. Ultrasound assessment of these parameters is demonstrably superior to digital examination for predicting successful vaginal delivery.5
Navigating the “Slow Progress” Plateau
When labor arrests or slows, POCUS provides objective data to guide the next clinical decision. Transperineal ultrasound can allow for the measurement of two validated parameters: the Angle of Progression (AoP) and the Head-Perineum Distance (HPD).7 These measurements provide quantifiable thresholds that digital examination cannot offer.
Clinical Insight: Research shows that the likelihood of cesarean section increases significantly when HPD exceeds 50 mm or AoP falls below 100°.8 Having these measurements available in real time enables more confident, evidence-based decision-making regarding augmentation, operative intervention, or expectant management.
Supporting Safer Neuraxial Anesthesia
One of the most impactful and often overlooked POCUS applications in L&D is facilitating epidural and spinal anesthesia placement. Obstetric patients frequently present with anatomic challenges (obesity, scoliosis, prior spinal surgery, or edema) that make traditional landmark-based techniques difficult. Ultrasound pre-procedure scanning to identify the optimal intervertebral space and estimate depth to the epidural space has been shown to significantly improve first-pass success rates and reduce the number of needle passes required.
A systematic review and meta-analysis published in The BMJ found that ultrasound guidance for epidural catheterization reduced the risk of failed placement and traumatic procedures compared with the conventional palpation technique.9 Similarly, a prospective study demonstrated that ultrasound imaging facilitates spinal anesthesia in patients with challenging surface landmarks, reducing procedural time and patient discomfort.10 For patients in active labor who may not tolerate prolonged positioning or repeated needle attempts, these benefits translate directly into improved patient experience and safety. Ultimately, data is clear that preprocedural ultrasound increases first-pass success by the order of almost 50%.11
Gastric Assessment and Aspiration Risk
Pulmonary aspiration pneumonitis (Mendelson’s syndrome) remains one of the most feared complications of obstetric anesthesia. All laboring patients are considered to have a full stomach, but the degree of risk varies and is often unknown at the time of urgent intervention. Gastric POCUS, using a standardized two-position assessment of the antrum, can allow anesthesia providers to qualitatively and semi-quantitatively evaluate gastric content and volume at the bedside.12
A standardized gastric ultrasound protocol can differentiate an empty stomach from one containing liquid or solid material, enabling more nuanced anesthetic planning – particularly when transitioning from neuraxial to general anesthesia for an emergent cesarean delivery. This application has gained traction as part of a comprehensive pre-anesthetic POCUS evaluation in the obstetric population.
Postpartum Vigilance: Scanning for Retained Products of Conception
The utility of POCUS does not end with delivery. The postpartum period – the “fourth trimester” – carries its own set of risks, most notably Retained Products of Conception (RPOC). Excessive bleeding, pain, or fever are red flags, but a definitive diagnosis is required to avoid unnecessary surgical intervention. POCUS, particularly when combined with Doppler imaging, plays a pivotal role in this differential.
The Power of Doppler: When evaluating these suspected masses, assessing intrauterine vascularity is key. Research indicates that true RPOC is highly vascularized: in one study, only 18% of retained tissues were avascular, while 21% had minimal vascularity, 43% moderate vascularity, and 18% marked vascularity.13 The advanced Doppler capabilities (PW, Color, and Power Doppler) found on the Kosmos Lexsa or Torso-One probes may enable clinicians to visualize blood flow within intrauterine masses, providing critical information to guide management.
Avoiding Complications: A blind dilation and curettage (D&C) performed on a highly vascular RPOC carries a significant risk of massive hemorrhage.13 POCUS allows for a more conservative and individualized approach – such as using uterotonics to encourage natural expulsion when vascularization is absent or minimal – reserving surgical intervention for high-risk cases.
The Kosmos Advantage:
Cart-Level Power at the Bedside
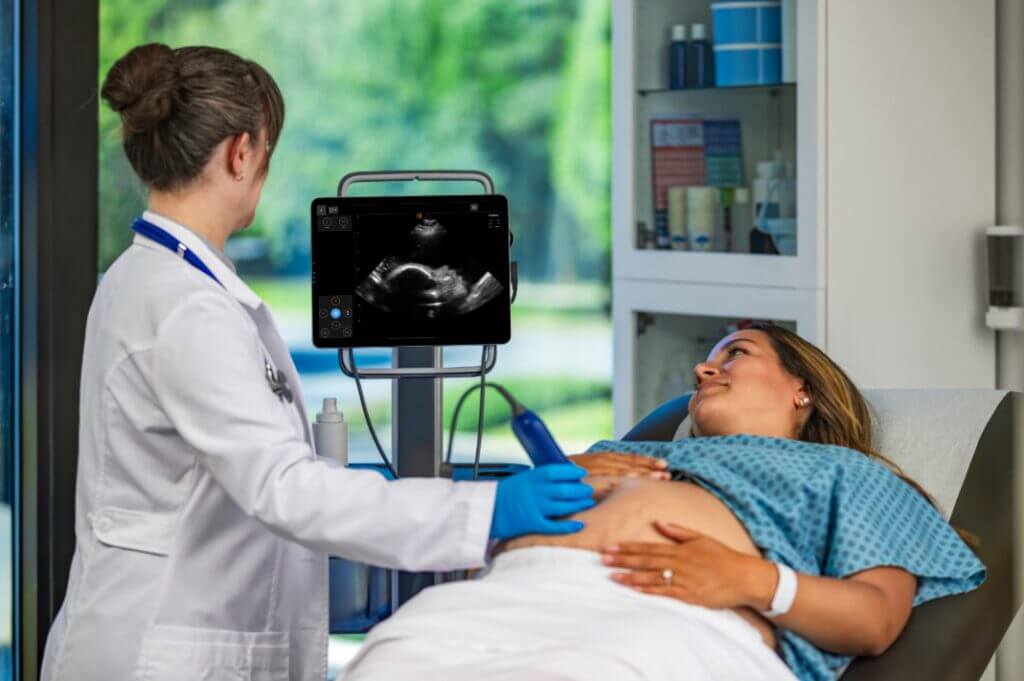
In a busy L&D unit, space is at a premium and time is of the essence. Traditional cart-based systems may often be too bulky to maneuver quickly during an emergency, such as a suspected placental abruption or uterine rupture. The Kosmos Plus configuration offers a “High-Value Hybrid” solution that addresses these operational realities:
Diagnostic Quality: Kosmos utilizes gold-standard PZT crystal technology to provide images that rival traditional, much more expensive echo and OB machines, ensuring clinicians are not compromising on image resolution at a critical moment.
Wired Reliability: Unlike wireless handhelds that can suffer from signal interference or battery failure in the probe itself, Kosmos uses a secure cabled connection to ensure the scan is not interrupted at a critical moment.
Infection Control: In an environment where contaminated gel and probes can contribute to infections, Kosmos probes are compatible with high-level disinfection systems like Trophon, meeting the stringent standards required for obstetric and gynecologic use.
Summary: POCUS Applications in Labor & Delivery
| Phase of Care | Clinical Utility | POCUS Application | Key Advantage |
|---|---|---|---|
| Admission | Triage & Assessment | Transabdominal fetal survey | Identifies malpresentation and unknown complications early |
| First/Second Stage | Monitoring Progress | Transperineal AoP & HPD measurement | Predicts delivery outcome and guides augmentation decisions |
| Anesthesia Placement | Neuraxial Guidance | Pre-procedure spinal/epidural scan | Improves first-pass success, reduces needle passes |
| Pre-Operative | Aspiration Risk | Gastric antrum assessment | Guides anesthetic planning for emergent cesarean delivery |
| Instrumental Delivery | Safety Confirmation | Head station & position verification | Prevents fetal/maternal injury from misapplied instruments |
| Postpartum | RPOC Detection | Color/Power Doppler[1] intrauterine survey | Evaluates vascularity to guide surgical vs. medical management |
By integrating POCUS into the standard of care across all phases of the labor and delivery encounter – from admission through the fourth trimester – L&D units can move toward a more objective, data-driven model that prioritizes patient safety, reduces unnecessary intervention, and closes the gap between what clinicians feel and what they can now reliably see, ultimately converting uncertain physical exam findings into objective, reproducible information at the bedside, supported by guidelines and evidence.[2] 14
References
- Sargın MA, Ilter PB, Kayabasoglu F, et al. It is time for midwives to perform intrapartum ultrasonography for fetal head station, position and cervical dilation. J Matern Fetal Neonatal Med. 2025;38(1):2493192 . doi:10.1080/14767058.2025.2493192
- Greenstein Y, Bhatt A, Vragovic O, Bhatt S, Jain S. Usefulness and training of point-of-care ultrasound in obstetric emergencies. J Ultrasound Med. 2019;38(11):2977–2983.
- Ghi T, Eggebø T, Lees C, et al. ISUOG Practice Guidelines: intrapartum ultrasound. Ultrasound Obstet Gynecol. 2018;52(1):128-139. doi:10.1002/uog.19072
- Akmal S, Tsoi E, Howard R, Osei E, Nicolaides KH. Investigation of occiput posterior delivery by intrapartum sonography. Ultrasound Obstet Gynecol. 2004;24(4):425–428.
- Rozenberg P, Porcher R, Salomon LJ, Boirot F, Morin C, Ville Y. Comparison of the learning curves of digital examination and transabdominal sonography for the determination of fetal head position during labor. Ultrasound Obstet Gynecol. 2008;31(3):332–337.
- Dall’Asta A, Melito C, Ghi T. Intrapartum ultrasound guidance to make safer any obstetric intervention: fetal head rotation, assisted vaginal birth, breech delivery of the second twin. Clin Obstet Gynecol. 2024;67(4):730-738. doi:10.1097/GRF.0000000000000891
- Barbera AF, Pombar X, Perugino G, Lezotte DC, Hobbins JC. A new method to assess fetal head descent in labor with transperineal ultrasound. Ultrasound Obstet Gynecol. 2009;33(3):313–319.
- Tutschek B, Braun T, Chantraine F, Henrich W. A study of progress of labour using intrapartum translabial ultrasound, assessing head station, direction, and angle of descent. BJOG. 2011;118(1):62–69.
- Shaikh F, Brzezinski J, Alexander S, et al. Ultrasound imaging for lumbar punctures and epidural catheterisations: systematic review and meta-analysis. BMJ. 2013;346:f1720.
- Chin KJ, Perlas A, Chan V, Brown-Shreves D, Koshkin A, Vaishnav V. Ultrasound imaging facilitates spinal anesthesia in adults with difficult surface anatomic landmarks. Anesthesiology. 2011;115(1):94–101.
- Young B, Onwochei D, Desai N. Conventional landmark palpation vs. preprocedural ultrasound for neuraxial analgesia and anaesthesia in obstetrics – a systematic review and meta-analysis with trial sequential analyses. Anaesthesia. 2021;76(6):818-831. doi:10.1111/anae.15255
- Van de Putte P, Perlas A. Ultrasound assessment of gastric content and volume. Br J Anaesth. 2014;113(1):12–22.
- Matijevic R, Knezevic M, Grgic O, Zlodi-Hrsak L. Diagnostic accuracy of sonographic and clinical parameters in the prediction of retained products of conception. J Ultrasound Med. 2009;28(3):295-299. doi:10.7863/jum.2009.28.3.295
- Rizzo G, Ghi T, Henrich W, et al. Ultrasound in labor: clinical practice guideline and recommendation by the WAPM-World Association of Perinatal Medicine and the PMF-Perinatal Medicine Foundation. J Perinat Med. 2022;50(8):1007-1029. doi:10.1515/jpm-2022-0160
Additional References
Q&A: Enhancing Patient Safety in Labor and Delivery with Point-of-Care Ultrasound
It refers to the shift of point-of-care ultrasound from an emergency “rescue” tool to a routine bedside assessment. It provides objective, real-time data that complements traditional physical exams, much like checking blood pressure or heart rate.
Digital exams are subjective and have inaccuracy rates between 20% and 70%. Ultrasound provides reproducible, objective measurements of fetal head position and station, which digital exams often misidentify.
Kosmos offers “cart-level” diagnostic quality (using PZT crystal technology) in a portable format. Unlike wireless handhelds, its cabled connection prevents signal interference, and the probes are compatible with high-level disinfection systems like Trophon.