What Is the “Best” Point-of-Care Ultrasound? A Clinician-Centered Framework
Search for “best point-of-care ultrasound” and the results are often dominated by product rankings and technical specification sheets. However, for clinicians, educators, and hospital leadership, these metrics rarely capture the reality of clinical practice. This article establishes a decision framework to help clinicians interpret the landscape of Point-of-Care Ultrasound (POCUS) devices. Rather than ranking brands, it defines “best” based on the variables that impact patient care: clinical context, user experience, and workflow integration. In other words, “best” is context-dependent, defined by clinical needs, user experience, and workflow integration – rather than raw hardware.1
Table of Contents
New Consensus: “Best” Defined by Workflow, Not Specs
In April 2024, the Society of Point of Care Ultrasound (SPOCUS) convened a multidisciplinary panel of experts to establish the first universal “best practices” for POCUS. Their consensus of 57 statements across 8 domains challenges the traditional way ultrasound systems are evaluated.
The panel acknowledged that POCUS has grown in a “grass-roots” pattern with a lack of standardization. Because of this, they concluded that good practices – and by extension, “best” systems – are not defined by raw hardware metrics but by “the subjective perception of a POCUS workflow that is efficient, safe, and ethical for clinicians, learners, and patients”.
In practical terms, this means workflow trumps specifications when judging an ultrasound device. A machine with the highest frequency probe or fanciest imaging modes could still be suboptimal if it doesn’t fit the clinical context. For example, a device might produce beautiful images, but if it’s too cumbersome in a code blue scenario, it’s not the “best” for that context. As the SPOCUS panel put it, efficiency, safety, ethical use, and things like ease-of-use, proper documentation, and patient privacy define the ideal POCUS setup.
When evaluating a system, this shifts the question from “Which machine has the highest frequency?” to “Which machine supports an efficient, safe, and ethical workflow?”
The Infrastructure of “Best”: Archiving and Safety
One of the most significant findings from the consensus is the critical role of infrastructure. The best ultrasound image is useless if it cannot be securely stored, reviewed, and documented.
- Archiving is Non-Negotiable: The panel overwhelmingly agreed (95.7%) that systems must have infrastructure for uploading and archiving images. The “best” POCUS device is one that seamlessly integrates with digital radiology systems, avoiding the “phantom scan” that lives only on the machine and never enters the patient record, a major problem considering almost 50% phantom scan rate in studies, leading to care gaps.2
- Safety and Hygiene: Device hygiene is a major workflow constraint. The experts emphasized that devices must be easily cleaned between every patient encounter, and that extra supplies (like gel packets and catheters) stored on the machine can become contamination vectors. A system designed with infection control in mind – easy-to-clean glass surfaces versus complex buttons – is often the “better” choice for high-acuity environments. In this context, a recent study demonstrated almost 20% prevalence of drug-resistant bacteria on ED transducers even with “standard” wipedowns, highlighting the hygiene factor in device choice.3
The Role of AI and Standardization
Perhaps the biggest challenge in defining the “best” ultrasound is the human factor and associated interoperator variability. A device that works well for an expert but confuses a novice is a liability, particularly considering that skill development is typically non-linear.
Modern POCUS systems with integrated AI guidance fit this need by:
- Supporting Standardization and Reducing Training Burden: Helping users acquire standard views without years of “knobology” training.
- Ensuring Quality Assurance: The panel recommended that, whenever possible, POCUS studies should be reviewed by experts for quality assurance. AI-driven systems that automate image labeling and quality grading can act as a force multiplier for this review process. In this sense, studies have shown that AI-integration has led to almost 95% compliance with POCUS documentation.4
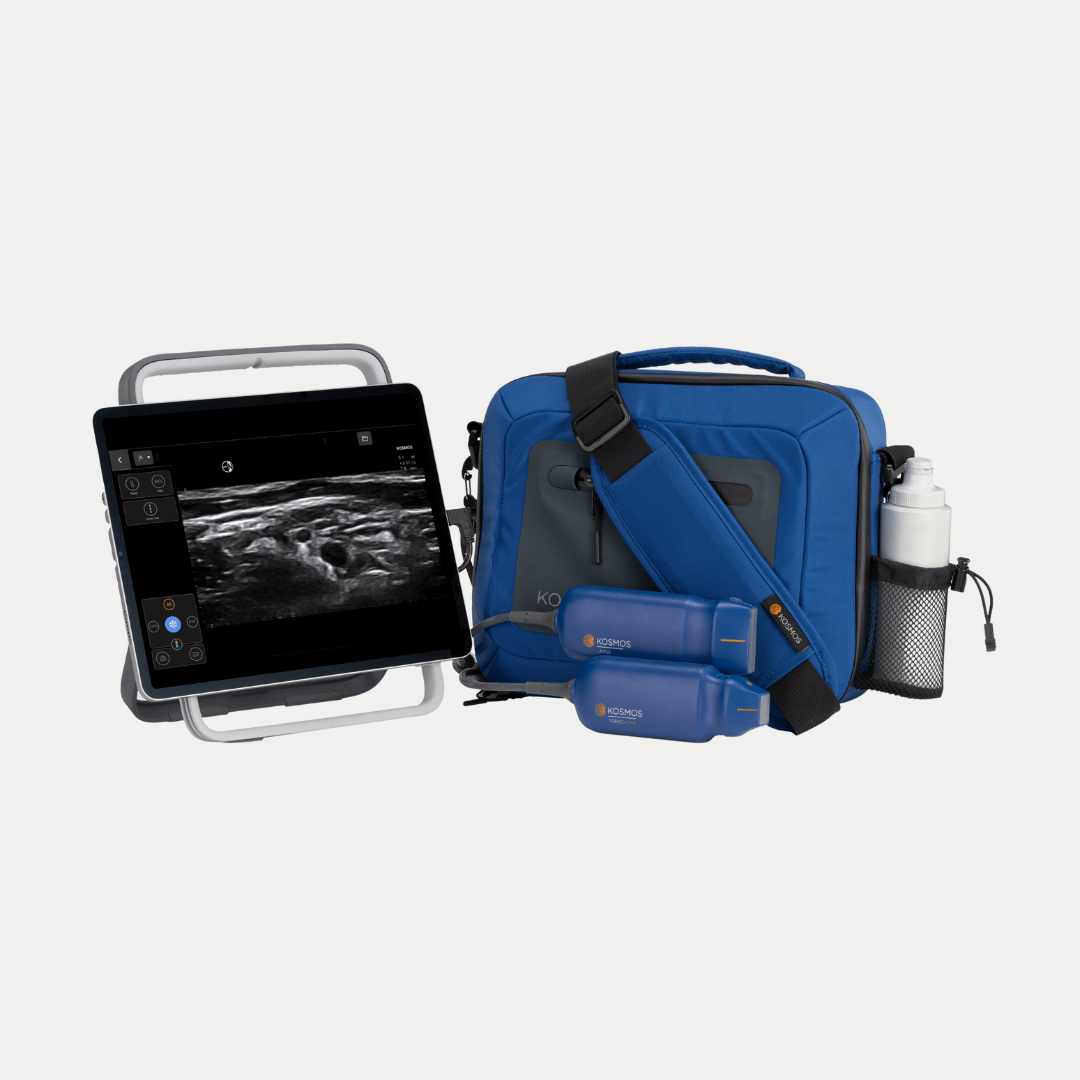
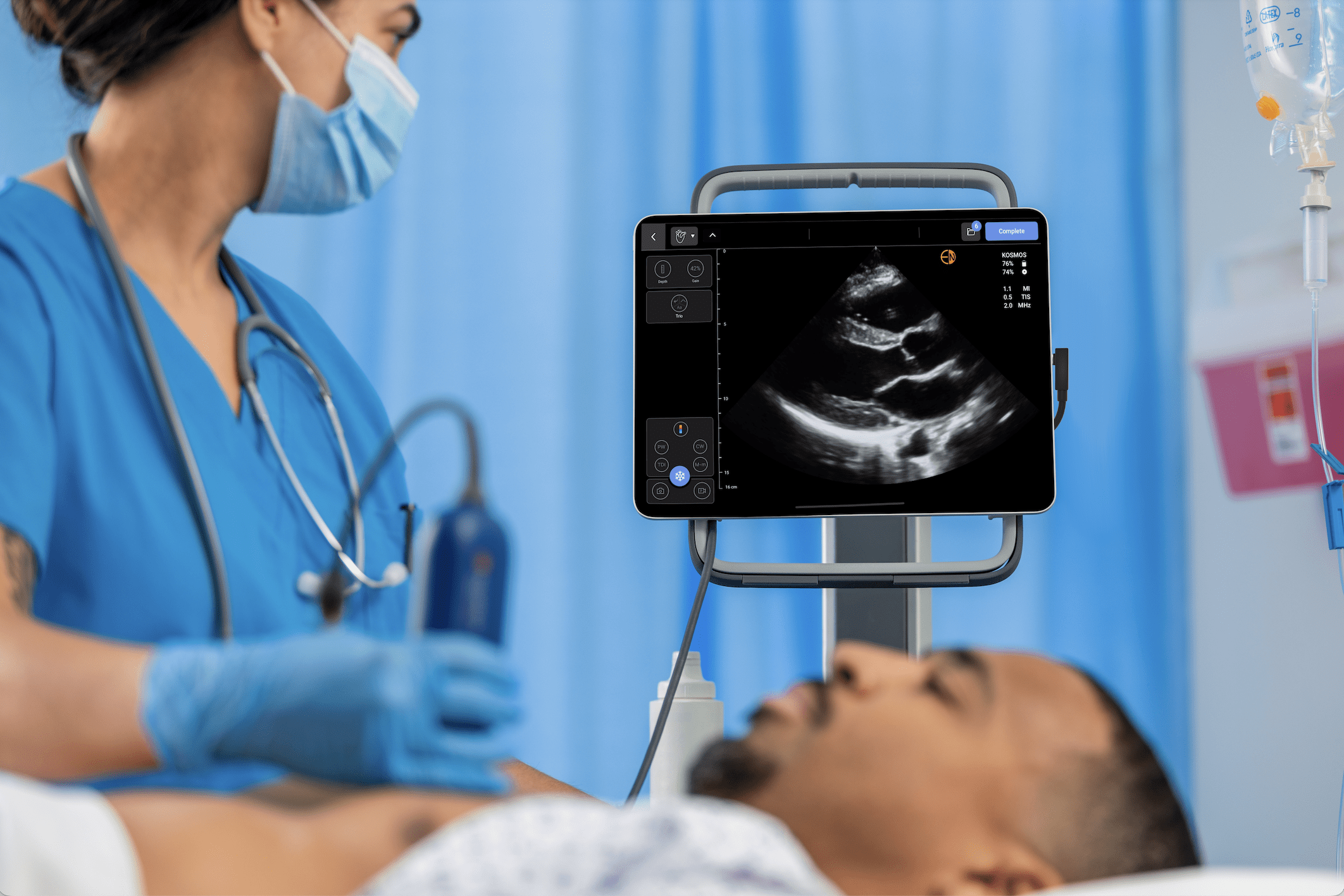
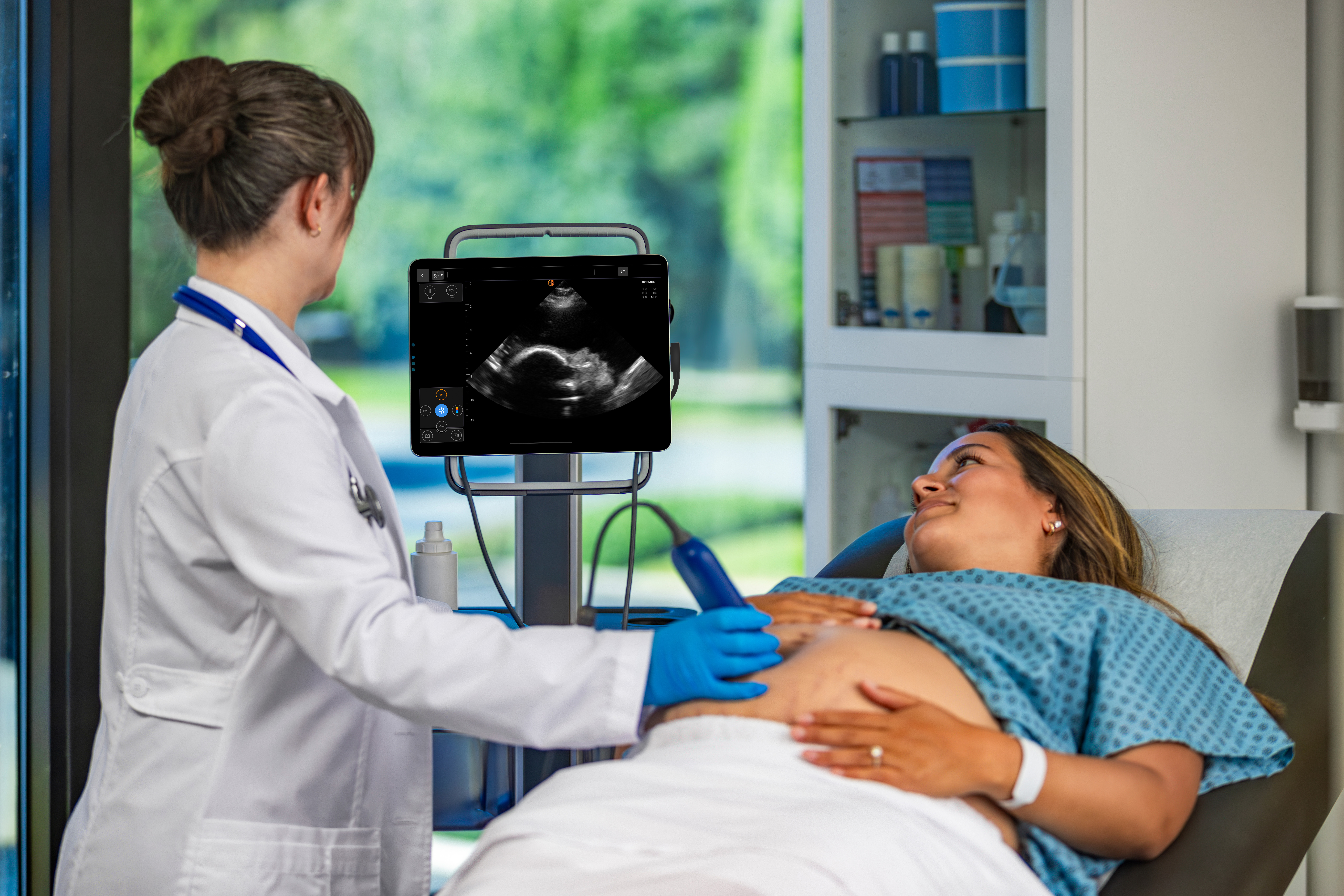
At EchoNous, we designed the Kosmos system to align with this exact framework – prioritizing workflow efficiency, seamless system design, and AI-assisted capabilities to improve the experience of the POCUS device user.
References
- Oto B, Baeten R, Chen L, et al. Best Practices for Point of Care Ultrasound: An Interdisciplinary Expert Consensus. POCUS Journal. 2024;9(1):95-108. DOI: 10.24908/pocus.v9i1.17240.
- Boivin Z, Dwyer KH, Pare JR, et al. Prevalence of ghost scans in point-of-care ultrasound for trauma patients: a multicenter study. Am J Emerg Med. 2026;99:354-358. doi:10.1016/j.ajem.2025.10.043
- Yamanaka T, Yamamoto R, Yajima K, et al. Bacterial contamination of ultrasound probes in emergency departments: a multi-centre observational study. J Hosp Infect. 2025;163:23-29. doi:10.1016/j.jhin.2025.03.017
- Rong K, Chimileski B, Kaloudis P, Herbst MK. Impact of an epic-integrated point-of-care ultrasound workflow on ultrasound performance, compliance, and potential revenue. Am J Emerg Med. 2021;49:233-239. doi:10.1016/j.ajem.2021.06.009
- Narang A, Bae R, Hong H, et al. Utility of a deep-learning algorithm to guide novices to acquire echocardiograms for limited diagnostic use. JAMA Cardiol. 2021;6(6):624-632. doi:10.1001/jamacardio.2021.0185
- EchoNous. Kosmos chemical compatibility. EchoNous. Accessed February 19, 2026. https://echonous.com/resource/chemical-compatibility-guide_kosmos-platform_english-2
Q&A: Defining the Best POCUS
The panel concluded that because POCUS use varies so much by specialty, best practices are defined by a workflow that is “efficient, safe, and ethical” rather than by rigid hardware specifications or universal rules.
95.7% of the experts agreed that systems should have infrastructure for uploading and archiving images. Without this, scans cannot be shared with the treatment team or reviewed for quality, rendering even the highest-resolution image clinically isolated.
Not necessarily. The experts noted that skill acquisition is non-linear and varies by user. The ideal system is one that supports this learning curve, often through intuitive design or AI assistance, rather than one that requires a “PhD in physics” to operate.5
The panel highlighted that “secondary components” like control panels and storage bins must be disinfected after every patient. Systems with complex knobs or porous surfaces are harder to clean, making smooth, touch-based systems a “better” fit for infection-prone environments. So, a “best” system is one designed with infection control in mind, e.g. by having disposable gel packets, probe covers, and surfaces that tolerate robust disinfection. In short, the easier a machine is to keep clean, the better fit it is for environments like the ED, ICU, or wards where preventing infection is a daily challenge.6