Training, Credentialing, and Competency for Ultrasound-Guided Vascular Access
The benefits of ultrasound-guided vascular access (USGIVA) are well-documented. A 2024 meta-analysis found that when nurses use ultrasound guidance, the odds of achieving successful IV placement on the first attempt are nearly three times higher than with traditional techniques.1 However, achieving these improved outcomes, along with reduced complications and enhanced patient satisfaction, depends heavily on one critical factor: operator training and competency.
Ultrasound-guided vascular access is a skill-based procedure requiring both technical proficiency for needle guidance and cognitive skills for image interpretation. To ensure safety and consistency, healthcare organizations must implement structured training, credentialing, and ongoing competency assessment programs. This article outlines the core elements of a successful program for building and maintaining clinical competency in USGIVA.
Table of Contents
- Training, Credentialing, and Competency for Ultrasound-Guided Vascular Access
- Foundational Knowledge: The Didactic Component
- Hands-On Skill Development: Simulation and Practice
- Clinical Integration: Supervision and Credentialing
- The Role of Technology in Modern Training
- Q&A: Ultrasound-Guided Vascular Access (USGIVA) Training
- References
- Interested in discovering Kosmos for Vascular Access? Connect with our team today!
Foundational Knowledge: The Didactic Component
An effective training program must begin with a solid grasp of the principles behind the image on the screen. This foundational didactic education instills a deeper understanding of ultrasound physics, “knobology” (machine settings), orientation and transverse/longitudinal views alongside image optimization. This knowledge is what allows a clinician to troubleshoot a poor image, adjust settings, and use features like Doppler to definitively distinguish a compressible vein from a non-compressible, pulsatile artery as well as be able to spatially puncture the vein either in plane or out of plane.
This theoretical knowledge is then applied to anatomy and structure identification. Operators must learn to reliably interpret the grayscale landscape of the screen, recognizing not just the target vessel but also the surrounding structures that must be avoided, such as nerves and fascia as well as the caliber and appropriateness of the vein for the catheter.
Hands-On Skill Development: Simulation and Practice
Once the foundational concepts are in place, the focus shifts to hands-on skill development, where clinicians translate theoretical knowledge into procedural confidence. This journey begins with simulation, a crucial step for developing the muscle memory required for precise needle guidance in a low-stakes environment.
Trainees practice on vascular access phantoms—lifelike models that simulate human tissue and vessels—to master the two primary needle guidance techniques:
- In-plane technique, where the needle is inserted parallel to the ultrasound probe, allowing for visualization of its entire length.
- Out-of-plane technique, where the needle enters perpendicular to the probe and is tracked as a dot in cross-section.
Supervised practice with real-time feedback from an experienced instructor accelerates this learning process, correcting minor errors in probe handling or needle angle before they become ingrained habits.
Clinical Integration: Supervision and Credentialing
After demonstrating proficiency in a simulated setting, the clinician transitions to performing procedures on patients under supervision. This is the most critical phase of training, where skills are refined in the dynamic and variable environment of real-world clinical care.
This supervised practice is the final step before credentialing, the formal process by which an institution verifies that a practitioner has met the minimum standards to perform USGIVA procedures independently. While specific requirements vary, they are guided by recommendations from leading healthcare organizations like the Infusion Nurses Society (INS) and the American College of Emergency Physicians (ACEP).
Competency is not static; it must be maintained over time through ongoing quality assurance programs, which can include periodic skills reassessments and peer review. As POCUS proponent Dr. Josè Pinto notes, a supportive community is crucial for ongoing skill refinement and sharing experiences.
The Role of Technology in Modern Training
The landscape of medical technology is constantly evolving. Modern ultrasound systems, with improved portability and more intuitive interfaces, are becoming integral to daily clinical practice. These advancements empower more clinicians to adopt this essential skill, ultimately expanding access to safer and more effective care.For institutions building a training, credentialing, and competency program for vascular access, choosing the right ultrasound system is a foundational step.
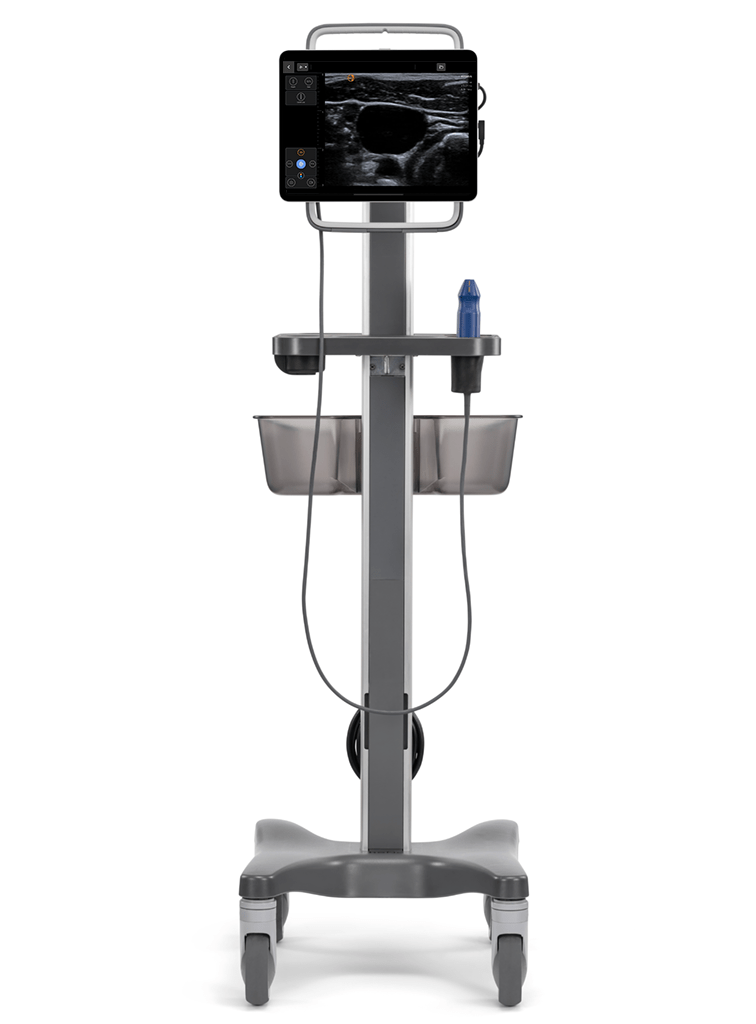
The Kosmos system by EchoNous is engineered to support clinicians at every stage of their learning journey. Its high-quality 2D compound imaging provides the exceptional clarity needed for trainees to confidently identify anatomy and visualize the needle path, flattening the learning curve and helping improve procedural safety. Advanced Color and Pulsed Wave Doppler capabilities make it easier to teach the critical skill of differentiating between arterial and venous structures, a cornerstone of competency. By providing an intuitive and powerful imaging platform, Kosmos helps streamline the entire training and credentialing process, ensuring a consistent standard of care. Equip your team for success—connect with a clinical product expert to see how Kosmos can enhance your vascular access program today.
Q&A: Ultrasound-Guided Vascular Access (USGIVA) Training
A 2024 meta-analysis found that when nurses use ultrasound guidance, the odds of achieving successful IV placement on the first attempt are nearly three times higher than with traditional techniques.
USGIVA is a “skill-based procedure requiring both technical proficiency for needle guidance and cognitive skills for image interpretation.”
Healthcare organizations should implement structured training, credentialing, and ongoing competency assessment programs.
It is the foundational education that instills “a deeper understanding of ultrasound physics, ‘knobology’ (machine settings), orientation and transverse/longitudinal views alongside image optimization.”
The journey begins with simulation in a “low-stakes environment.” Trainees practice on “vascular access phantoms”—lifelike models that simulate human tissue and vessels.
Once a clinician has shown they are proficient in the simulated environment, they move on to the most important stage of their training: performing supervised procedures on actual patients.
No. Competency is not static; it must be maintained over time through ongoing quality assurance programs.
References
- Tian Y, Zhong Z, Dougarem D, Sun L. The ultrasound-guided versus standard technique for peripheral intravenous catheter placement by nurses: A systematic review and meta-analysis. Heliyon. 2024;10(9):e30582. https://pmc.ncbi.nlm.nih.gov/articles/PMC11098833/